Overview
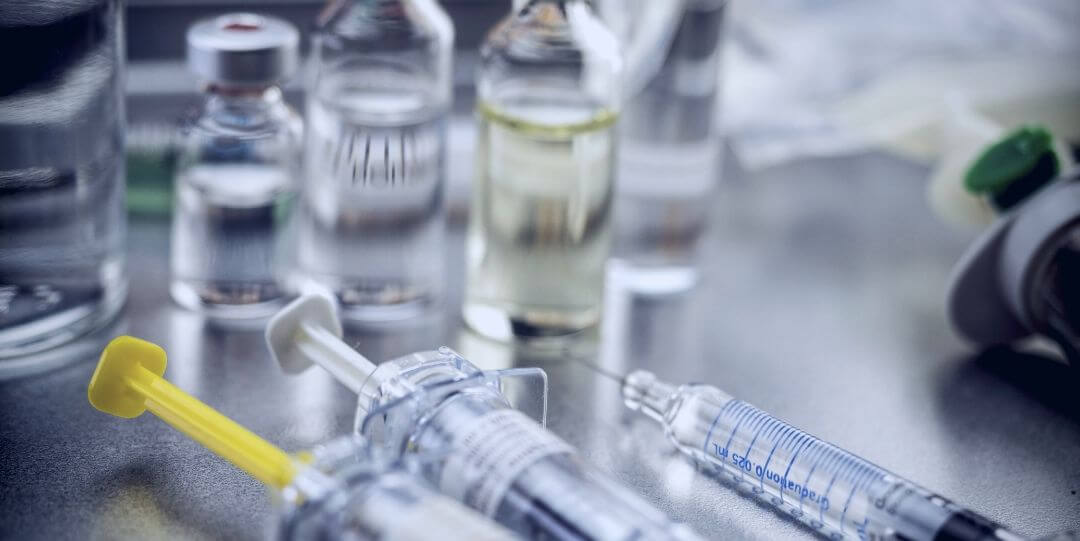
Antimalarial drugs are associated with severe and alarming side effects such as serious psychiatric and nerve problems, hallucinations, vaginal infections, etc. Therefore, it is important to take precaution while taking these medications. However, malaria is a serious disease and those who are traveling to areas where malaria is a threat should consider taking antimalaria drugs to prevent and suppress malaria symptoms. Discuss the risks of taking and the risks of not taking antimalarial drugs with a healthcare professional who is experienced in this field.
The health care provider will determine which antimalarial drug is best based on where you will be traveling (and potentially exposed to malaria mosquitoes) and your health condition.
Common Names:
- Chloroquine (Aralen)
- Primaquine
- Mefloquine (Lariam)
- Combination of atovaquone and proguanil (Malarone)
- Doxycycline
Side Effects and What to Do About Them
Chloroquine (Aralen)
Side effects are normally mild and include: headache, loss of appetite, diarrhea, upset stomach, stomach pain, skin rash or itching, hair loss, mood or mental changes.
People who have psoriasis should take precaution when using Chloroquine because it may increase the severity of the disease. A Syracuse University study found that using Chloroquine excessively for a long period of time could be dangerous. Prolonged use of this medication could potentially lead to unwanted and fatal side effects such as gastrointestinal distress, chemical harm to the heart and death. Additionally, Chloroquine is not a drug that should be taken for last minute travelers. In order for this drug to be effective, travelers should start this medication 1 – 2 weeks prior to taking their trip.
Atovaquone/Proguanil (Malarone)
Serious and unusual reactions are: blistering, peeling, red skin rash, fever, chills, headache, cough, sore throat, body aches, seeing or hearing things that are not there, seizures, sores or white patches on your lips, mouth, or throat.
Less serious side effects: cough, headache, mild skin rash or itching, nausea, vomiting, diarrhea, stomach pain, loss of appetite, weakness, dizziness.
People who have a history of kidney failure should not take Atovaquone. Additionally, women who are pregnant or breastfeeding a child less than 5 pounds should also avoid this medication.
Doxycycline:
Serious side effects can include: blistering, peeling, red skin rash, burning, pain, or irritation in your upper stomach or throat, diarrhea that may contain blood, fever, chills, cough, runny or stuffy nose, sore throat, body aches, joint pain, fever, rash, and unusual tiredness or weakness, severe headache, dizziness, vision changes, sudden and severe stomach pain, nausea, vomiting, lightheadedness.
Less serious side effects: darkening of your skin, scars, teeth, or gums; sores or white patches on your lips, mouth, or throat.
Mothers to be and children under 8 years old should not take Doxycycline. This medication can cause vaginal yeast infections, an upset stomach and can increase sensitivity to the sun. Doxycycline has also been found to decrease contraceptive efficacy.
Primaquine
Serious side effects: dark urine, fainting, dizziness, lightheadedness, trouble breathing, tiredness, uneven heartbeat, yellow skin or eyes.
Common side effects are nausea, upset stomach, vomiting, loss of appetite, heartburn, and abdominal cramps.
People with a glucose-6-phosphatase dehydrogenase (G6PD) deficiency (a disorder where medications, infections, or other stressors causes red blood cells to break down) should not take Primaquine. This medication should not be used by pregnant women or women who are breastfeeding, unless the child has been checked for G6PD deficiency. Additionally, anyone living in an area known to have Plasmodium vivax malaria should be tested before administration of Primarquine.
Mefloquine (Lariam)
Serious side effects include: blistering, peeling, or red skin rash, dark-colored urine or pale stools, nausea, vomiting, loss of appetite, pain in your upper stomach, yellow skin or eyes. Faintness, dizziness, lightheadedness, balance problems, ringing in your ears. Fast, slow, pounding, or uneven heartbeat. Feeling confused, depressed, nervous, restless, or paranoid. Fever, chills, cough, sore throat, and body aches. Seeing, hearing, or feeling things that are not there. Unusual behavior or thoughts of hurting yourself.
Less serious side effects: diarrhea, vomiting, stomach pain, headache
Side effects associated with Lariam include anxiety, paranoia, hallucinations, depression, confusion, unusual behavior, dizziness, balance problems, convulsions, insomnia and psychiatric reactions.
The FDA applied a black box warning on Lariam’s label due to a serious risk of psychiatric and nerve side effects in 2013. The FDA updated the information on the label (pdf) to warn that neurologic side effects may persist or become permanent.
This drug is not intended for pregnant women or for patients who have experienced cardiac and liver conditions.
In 2013, CBS News reported that the Surgeon General’s Office of the Army Special Operations Command prohibited the use of Lariam because some soldiers were wrongly diagnosed with post-traumatic stress disorder when it was actually Lariam causing the psychological issues.
Drug interactions
Mefloquine may interact with other antimalarial drugs and antiseizure drugs. Additionally, Combining Chloroquine and Mefloquine may increase the risk of convulsions. The CDC warns against using Mefloquine and Lumefantrine together because a potentially fatal heart arrhythmia can result.
Chloroquine should not be used in combination with sotalol, amiodarone, or lumefantrine, or with the antiretroviral rilpivirine, because a potentially fatal heart arrhythmia can result.
For additional interactions between antimalarials and other medications, visit the CDC website.
Effectiveness & Considerations
Antimalarial drugs do not completely protect travelers from the parasite. Therefore, it is important that travelers combine the drugs with other recommended protective measures such as insect repellent, clothes that cover all parts of the body, sleeping in a space where mosquitos aren’t present or using insecticide treated sleeping nets. Additionally, it is important to take these medications with precaution because of possible drug interactions.
If malaria is contracted, read our story about a test to help avoid deadly side effects of the cure.
Alternatives to Antimalaria Drugs
Currently, there aren’t alternative antimalarial remedies or medications. However, there are precautions travelers can take to avoid the risk of malaria. According to the Center for Disease Control (CDC), travelers can avoid contact with mosquitoes by remaining in well-screened areas, using mosquito nets when sleeping, and wearing clothes that cover most of the body. Protection should be enforced first thing in the morning and during the evening.
Furthermore, insect repellent should be a staple product in a traveler’s suitcase and used on exposed skin. Travelers should purchase repellents that contain DEET (Diethylmetatoluamide), which is the most active and effective ingredient found in repellents. Read MedShadow’s article on bug repellents.
How They Work (Method of Action)
Antimalarial drugs are intended to treat and prevent malaria by killing the parasite in the liver or the bloodstream. It is important to keep in mind that antimalarial drugs only reduce your risk of infection by about 90%. Therefore, it is imperative that travelers take precautionary steps to avoid potentially hazardous mosquito bites. The type of medication and the duration will vary depending on the type of malaria parasite, the severity of the symptoms, age, and whether the traveler is pregnant.