The Centers for Disease Control and Prevention (CDC) recently announced that if you’re vaccinated and not in a large crowd, you don’t need to wear a mask outdoors. Some of us, though, may still want to wear one for another reason. Research suggests that the face covering may help reduce the allergy symptoms, like runny noses and itchy throats.
Allergy symptoms happen when your body recognizes something harmless, like pollen or dust known as an “allergen,” as potentially dangerous and mounts an immune response. While allergens like peanuts and pet dander persist year-round, many of us suffer from seasonal allergies, triggered by specific types of pollen that plants and trees release strictly during certain months of the year – often in spring.
Allergies can affect the skin, eyes, lungs and upper-respiratory pathways of your nose and throat.
Jeannie Kenkare, MD, chief medical officer of PhysicianOne Urgent Care, says, “Some people experience these allergies in the upper airways, with symptoms, such as watery eyes, runny nose, sneezing, nasal congestion, itchy eyes and scratchy throat. Others have more severe symptoms affecting the airways that lead to coughing, wheezing, shortness of breath and asthma. Some get symptoms affecting the skin, such as rashes, hives and redness. Seasonal allergies can also trigger pre-existing skin conditions, such as atopic dermatitis or eczema.”
Avoiding allergy catalysts works better than managing the symptoms. Here are some ways that can help you skip suffering from allergies this year.
Use A Mask to Block Pollen and Other Irritants
For the last year or so, wearing a mask has been reducing the amount of COVID-19 viral particles (SARS-COV-2 virions) you breathe in. It can also limit the amount of dust, pollen, dander and other allergens you inhale as well. The good news is that most of these allergens are much larger than the virus.
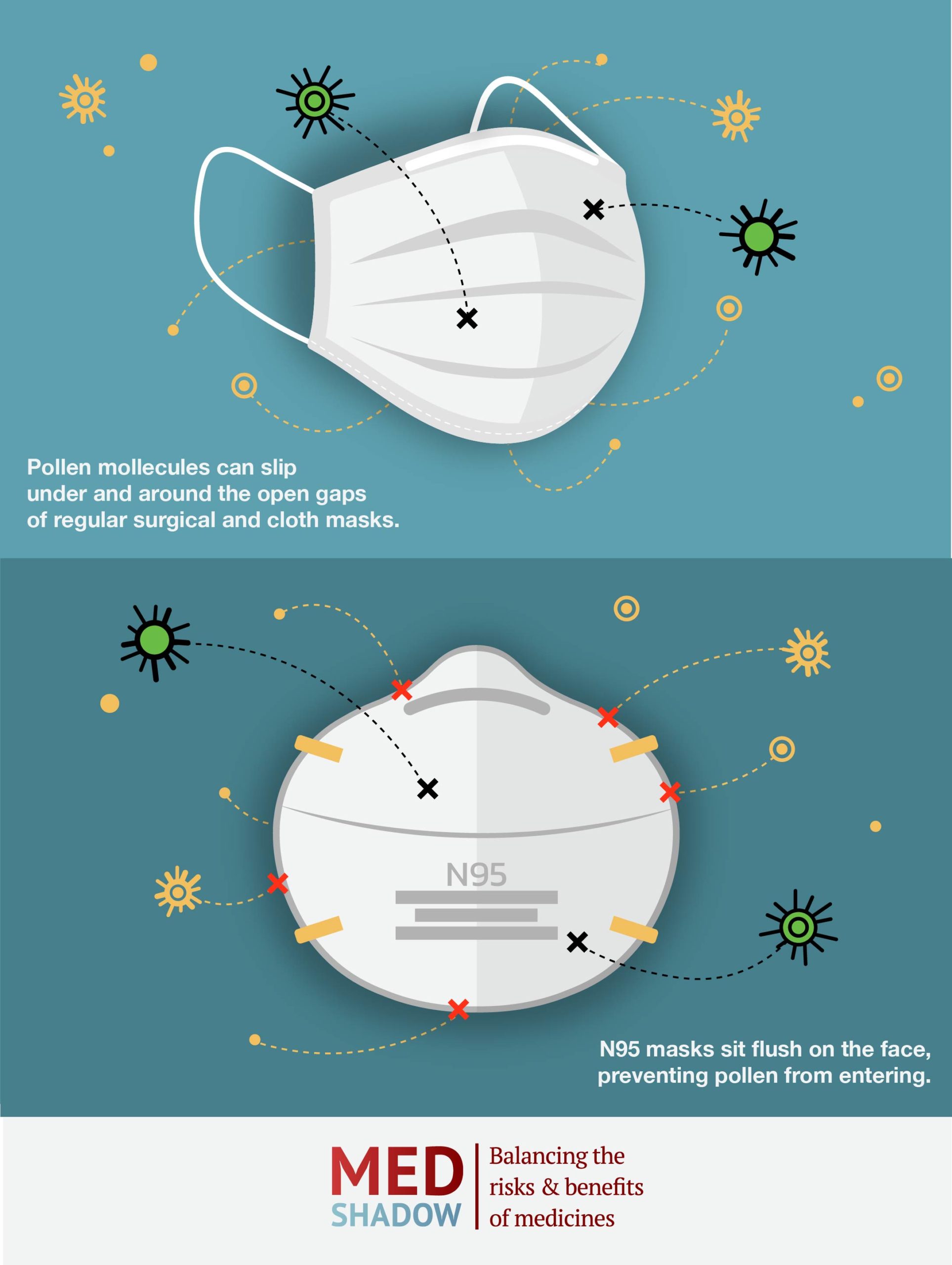
While a tight-fitting N95 is the most efficient of masks, most, including cloth and surgical ones, are likely to help. Most surgical masks block particles larger than 3 microns and N95s bar particles as small as 0.04 microns. Common allergens like fungal spores and pollen range from 2 to 100 microns. However, there are some allergens, like mold spores, that can be even smaller and penetrate masks. Ryan Smith, for example, who works in pest control where he is often exposed to grasses, pollens and pesticides, says he’s been wearing masks throughout the pandemic, but hasn’t noticed a difference in his allergy symptoms.
One study published in 2020 showed that 30% to 54% of nurses who wore either disposable surgical masks or N95s to protect themselves from COVID-19 reported fewer allergy symptoms.
Fit is the most important characteristic when choosing a mask to mitigate environmental allergies. An N95 mask that is snug against the skin around your nose and mouth will be far more effective than a face shield that only blocks particles blowing directly onto your face. Any spaces between your face and the mask are holes in which those particles can likely get in. The fewer particles you breathe in, the less severe your symptoms are likely to be.
Alternatives
To clear out your nasal passages, try a nasal saline spray or neti pot. “Peppermint oil is also great when inhaled, put in the bath, or in your tea, as it can help break up mucous secretions and reduce allergy symptoms related to mucus. Lemon oil is anti-inflammatory and increases salivation. Both properties reduce the congestion that occurs with seasonal allergies,” Smith says.
Smith says that breathing in the hot, humid air when he takes warm showers helps relieve his sinus pain, which is triggered by allergies.
Exposure Therapy
For some patients, regular exposure to tiny amounts of their allergen may help the body adjust. Two ways to get such exposure are through weekly allergy shots at your healthcare provider’s office or by eating local honey made during the time your allergies affect you. Local honey “contains trace amounts of local pollen carried by bees so your body can become familiar with local pollen and recognize it as less of a threat, leading to a lower allergic response,” says Shirin Peters, MD, founder of Bethany Medical Clinic in New York.
Keep Allergens Out of Your Home
The most effective way to reduce allergies, of course, is to make sure we don’t come in contact with allergens at all. While eliminating all the allergens from our lives is often impossible, there are many ways we can reduce our exposure and thus, limit our symptoms. One strategy is washing clothes immediately when you return home from being outside, to ensure you don’t deposit allergens on your furniture. Alternatively, you can try sealing the clothes in a bag until you can wash them. Check out this 2017 article in which the MedShadow staff discusses strategies, such as regular vacuuming and drying wet areas to prevent mold.
Hide From the Allergens
Monitor pollen counts outside by using apps or websites like breezometer.com. If you’re allergic to pollen, try to stay inside as much as possible on days when the counts are high and keep doors and windows closed. If you need to go out, you might consider wearing a mask.
If your allergies to outdoor allergens like pollen are still triggered when you’re indoors, Karkare suggests that you keep windows closed and consider adding a HEPA-filtration air purifier to your home or rooms. Peters says wearing a mask while cleaning around the house can reduce exposure to dust as well.
@savetimeshanThings I Wish I’d Known Sooner part 1 ##allergies ##allergytiktok ##allergycheck ##lifehacks ##cleaningtips ##cleaninghacks ##masktips ##cleaningtricks ##clean♬ Aesthetic – Xilo
If All Else Fails, Here’s the Lowdown on Drug Treatments
The most common treatment for allergies are antihistamines. They’re available both over-the-counter (OTC) and with prescriptions and come in many forms, such as tablets, liquids and creams.
Antihistamines block a chemical called histamine, that causes your blood vessels to constrict, leading to a runny nose and scratchy throat. Some patients may be instructed to use the drug daily, while others only take them when symptoms arise.
There are two generations of antihistamines. The first generation are older antihistamines that cross the blood-brain barrier more efficiently than the newer ones, and thus are more likely to cause certain side effects like drowsiness and constipation.
First-generation antihistamines include:
- brompheniramine (Children’s Dimetapp Cold)
- chlorpheniramine (Chlor-Trimeton)
- clemastine (Dayhist)
- cyproheptadine (Periactin)
- dexchlorpheniramine dimenhydrinate (Dramamine)
- diphenhydramine (Benadryl)
- doxylamine (Vicks NyQuil, Tylenol Cold and Cough Nighttime)
- hydroxyzine (Vistaril)
- phenindamine (Nolahist)
Second-generation antihistamines include:
- azelastine (Astelin)
- loratadine (Claritin)
- cetirizine (Zyrtec)
- desloratadine (Clarinex)
- fexofenadine (Allegra)
Side effects may be:
- Drowsiness
- Constipation
- Dry mouth, eyes and skin
- Nausea, abdominal pain
- Low blood pressure
- Increased heart rate
Using antihistamines long-term, especially the first-generation types, can cause other effects because they also block a neurotransmitter called acetylcholine. A 2015 study in JAMA suggested that taking antihistamines over time could increase your risk of dementia, which is sometimes characterized by a reduction in acetylcholine. Many drugs act on this neurotransmitter, so it’s important to tell your doctor or pharmacist if you’re using allergy medicines, even if they’re OTC.
If you’re using Zyrtec-D or Claritin-D, which are designed to treat congestion along with allergies, you may also experience an increased heart rate.
Nasal Corticosteroids
Nasal corticosteroids are sprayed into the nostrils to target inflammation caused by the allergen and to open airways.
Side effects are:
Nose bleeds
Eye pain or vision changes
Face swelling
Dizziness
Headaches
Singulair, With Caveats
Singulair is a leukotriene inhibitor. It’s the only drug in this class approved for treating allergies. More importantly, it is not considered a frontline treatment because, in some patients, it can cause anxiety, depression, insomnia and suicidal ideation. One MedShadow reader relayed her child’s harrowing story of experiencing rare psychiatric side effects after being prescribed the drug.






