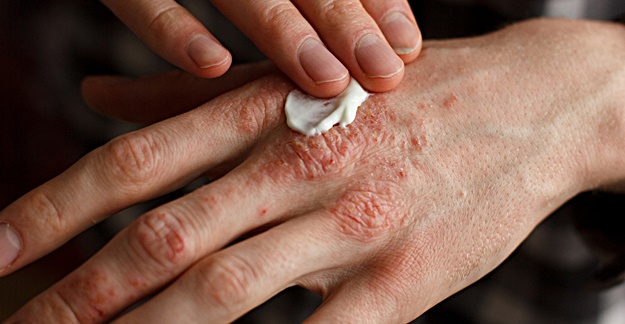
Eczema, also known as dermatitis, is a condition that causes red, inflamed, itchy rashes, and blistered, cracked patches of skin. People with eczema have very dry skin, which prevents the skin’s outer layer, the epidermis, from functioning properly as a protective barrier. Treating eczema is possible.
The most common type of eczema is known as atopic dermatitis, which is chronic eczema characterized by flares of disease followed by periods of clear skin. The causes of eczema are not known for sure but could include changes in genes, inappropriate immune reactions, or exposure to certain things in the environment, such as tobacco smoke or skincare products.
Eczema can feel like a moving target for people who live with it. They get control over one flare, only to have eczema redden and irritate another patch of skin. For some patients, changing their bathing and beauty habits, along with applying a thick moisturizer and topical corticosteroid ointments are enough.
Treating Eczema With Holistic Solutions
Moisturize First
American Academy of Dermatology (AAD) guidelines recommend using moisturizers first to combat the signature dry skin so characteristic of eczema. Moisturizers are considered a cornerstone of eczema management. Moisturizers relieve dry skin by combating water loss from the epidermis. Ingredients in common moisturizers include emollients, which lubricate the skin, occlusive substances, which prevent water from evaporating, and humectants, which hold onto water. Studies show that moisturizers containing any of these substances improve the dryness, itching, redness, and cracking of the skin.
Take a Bath
According to the AAD, there is not a lot of evidence that bathing offers benefits for people with eczema, but when done properly soaking or showering in warm water can help remove crust, allergens, and irritants from the skin. If water is left to evaporate on the skin it can worsen dry skin and trigger a flare. But moisturizing or applying a topical treatment immediately after bathing, while the skin is still wet, will add moisture to the skin.
The AAD recommends bathing in warm water up to once daily for five to ten minutes, then immediately moisturizing without toweling dry. For significantly inflamed skin, it may be helpful to soak in warm water for 20 minutes and immediately apply a topical anti-inflammatory treatment while the skin is still wet.
Wet Wrap Therapy
Wet wrap therapy is the application of a wet dressing to the inflamed area following bathing and moisturizing or after applying a topical medication. Dressings are made from a piece of cloth soaked in warm water, applied to the skin, and then covered with a dry dressing. The wet layer should be soaked again if it starts to dry out. Wet wraps can help improve symptoms by keeping skin moist and improving the effectiveness of topical treatments.
In addition to these simple steps, the National Institute of Allergy and Infectious Diseases suggests avoiding anything that triggers or worsens symptoms, such as wool, lanolin, strong soaps or detergents, stress or sudden changes in body temperature. Also, keep fingernails short and try not to scratch the skin. If nighttime scratching is a problem, consider wearing light gloves to bed.
Mind-Body
Using mind-body techniques to reduce stress may also help reduce symptoms of eczema. Research shows an association between eczema and anxiety and depression, with more severe eczema leading to greater depression. A small study in the journal ActaDV found that when people with eczema practiced progressive muscle relaxation (PMR) using a physical and mental component, they experienced improvements in itching and sleeping.
Researchers assigned two groups of people with eczema to either PMR along with conventional treatment, or conventional treatment alone. The PMR group practiced tensing and relaxing muscle groups over the arms, legs, face, abdomen, and chest. They tensed muscles for about 10 seconds, then relaxed for 20 seconds, twice a day for four weeks. For the mental component, they concentrated on the sensation of tension and relaxation.
Patients practicing PMR experienced a reduction in itching and sleep loss while the other group did not experience those improvements. The researchers suggest that PMR may be useful as an adjunct treatment, along with conventional therapy, for the management of eczema through the reduction of anxiety.
A study in the British Journal of Dermatology points to mindfulness — paying attention in the present moment without judging your thoughts or feelings — as a potential means of improving quality of life in people with eczema and other skin conditions. The researchers suggest that mindfulness interventions, including mindful meditation and cognitive behavioral therapy, may help improve social anxiety associated with visible skin conditions.
Topical Treatments
“Topical steroids are the mainstay of treating atopic dermatitis. They’ve been around for decades. They are generally inexpensive, and for the vast majority of patients, that’s how we start treatment,” explains dermatologist Amy Paller, MD, director of the Northwestern University Skin Biology and Diseases Resource-based Disease Research Center in Chicago.
However, some people with eczema find those first steps offer little relief. The topical corticosteroids either don’t help or seem to lose efficacy (become less effective) after a while. But before moving on to a more potent treatment, patients need to be sure they’re administering the steroid treatment properly and adequately. Research shows that often patients do not apply the treatments in proper amounts or as often as they should. Sometimes this is because they haven’t received adequate instructions from their doctor on how and when the steroids should be used, leading to improper use and poor response.
Also, patients may be concerned about the risks of using steroids on their skin, so they don’t stick to their regimen. “Topical steroids, while effective, have many side effects, especially when used long term,” says dermatologist Emma Guttman, MD, Ph.D., vice chair for research in the department of dermatology at the Icahn School of Medicine at Mount Sinai in New York City. Side effects of corticosteroids include skin irritations and thinning of the skin.
But even after following instructions and staying on top of their treatment protocol, some people still don’t get the relief they need from topical corticosteroids. For these people, new eczema treatments offer renewed hope.
When Corticosteroids Aren’t Enough
Dr. Paller acknowledges that corticosteroids aren’t good options for everyone. “Sometimes we have patients who can’t just intermittently apply steroids, clear their skin up, and use moisturizers. They are more chronic,” she says.
Jennifer Merrill, a resident of western Maine, is among those for whom eczema remains a frustrating puzzle. She’s had eczema since childhood. The 40-year-old managed to reduce eczema on her scalp by washing her hair less frequently and abstaining from hairspray – only to find that eczema moved to the skin around her lips, eyes, wrist, and stomach. A dermatologist prescribed a number of different creams, including topical corticosteroids.
“The steroids started to work in the beginning, but quickly things went from bad to worse,” she recalls.
A different dermatologist put Merrill on antibiotics and nonsteroidal prescription medication, Elidel (pimecrolimus).
“Things calmed down a bit, but I would get random flares. After about six months on antibiotics I went back, at which time she did a biopsy and the results were eczema,” she says. At that point, Merrill’s dermatologist gave her samples of a newer medication approved for use on eczema: Eucrisa (crisaborole).
“It has helped somewhat. Pretty much cleared up the patches on my wrist, has helped but not completely cleared my face, and has done nothing for my stomach. The area I need to use it the most now is around my lips. I’ve used it on my wrists and belly and felt no side effects, but when applied around my lips it burns and itches like crazy! After a few minutes, it will go away, but those first few are torture,” she says.
Nonsteroidal Options to Treat Eczema
Eucrisa was approved by the FDA in 2016 for use on eczema in people aged two and older and received approval for those as young as 3 months in 2020. A thin layer is applied to the affected areas twice daily.
Eucrisa has been shown to improve eczema symptoms safely, according to a review of the research on the ointment published in the December 2017 issue of the American Journal of Clinical Dermatology. According to the review, a small number of people using Eucrisa experience some pain at the site. A follow-up study in the journal Pediatrics a year later showed similar positive results and added a long-term improvement to the list of the drug’s benefits.
Eucrisa is indicated for mild to moderate eczema. It is essentially an anti-inflammatory that targets a specific enzyme in eczema that is causing inflammation.
Paller notes that Eucrisa is promising for areas of delicate skin, such as the skin on the face or close to the eyes, and adds that the ointment seems to be effective for hand and foot eczema as well.
People who use Eucrisa may find that they feel a burning or stinging at the site, says Paller. Some people can continue to use the ointment and find the unpleasant sensations go away – while others might have to switch to another option, she says. There’s currently no standard recommendation on how to reduce the burning sensations. In some situations, using a corticosteroid ointment to reduce the inflammation and then using a nonsteroidal ointment might help.
Elidel and Protopic are nonsteroidal creams used in people aged 2 years or older with mild to moderate eczema. Labels on Elidel and Protopic are both required to carry a black box warning due to the potential risk of cancer with long term use. As a result, these treatments are only recommended for people who can’t use other treatments, or whose eczema symptoms did not improve with other treatments.
Protopic’s black box includes a warning not to use the stronger 1% formulation in children between 2 and 15 years old. Only the .03% strength should be used by this age group. Also, neither Elidel nor Protopic is recommended for use longer than six weeks.
These topicals should be applied in a thin layer twice daily. They may cause burning, stinging or redness, and should not be used with occlusive dressings.
Dupixent (dupilumab) is an injection given under the skin every two weeks for people aged 6 years and older with moderate to severe eczema. Its use is limited to those who can’t take other therapies or whose eczema didn’t respond to topical treatments. Dupixent is often used along with topical corticosteroids.
Dupixent is in a class of drugs called monoclonal antibodies, proteins made in the lab that work like natural human antibodies in the body’s immune system. The most common side effects are injection-site reactions, conjunctivitis, and mouth or lip sores. If patients experience new or worsening eye symptoms such as redness, itching, pain or visual changes, they should consult their doctor immediately.
Dupixent, as well as other nonsteroidal treatments, can be pricey. Two injections of Dupixent, which is what you’ll need for one month of treatment, lists at about $3,100. One month of treatment with Eucrisa, or one 60g tube, costs about $650. A tube of Elidel costs around $360, but there is a generic version available for about $220. And a tube of Protopic costs about $350, with a generic cost of about $250. On the other hand, a tube of topical corticosteroids can cost less than $10.
However, most people do not pay full price for any of these treatments. If you don’t have insurance to help cover your treatments, check with the drug’s manufacturer. Pharmaceutical companies often have programs to help reduce the cost of their products.
Overall, atopic dermatitis is estimated to cost the country $5 billion dollars annually. This annual cost includes the cost of treatment and hospitalization, as well as the cost of lost work and productivity, according to an article published in Advances in Experimental Medicine and Biology in 2017. The most cost-effective strategy for eczema management may be the preventive use of moisturizers.
Paller points out that the arrival of newer eczema treatments such as Eucrisa, Elidel, Protopic, and Dupixent is just the tip of the iceberg — she expects researchers in future years to develop more treatments based on an increasingly nuanced understanding of how eczema works.