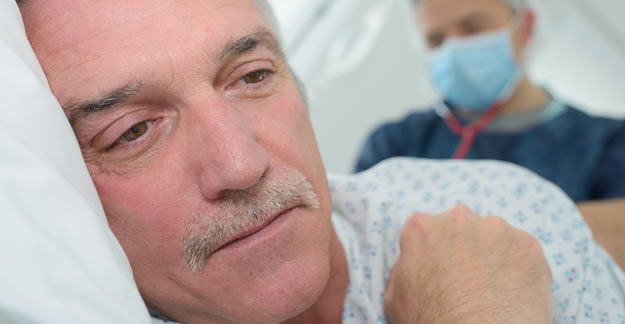
PSA testing for prostate cancer is controversial. As a screening tool it is inaccurate, hard to interpret and most often leads to no action.
Watchful waiting or active surveillance is now recommended by many physicians because of how slowly prostate cancer most often grows. There is very little reason for a healthy man, who is not in the high risk group, to take the test.
However, if you are a man in a high risk group (see below for who falls into high risk), the early treatment a positive PSA screening test triggers could save your life. Prostate cancer has almost no symptoms, but when symptoms appear, it’s then often too late for significant care and recovery. The PSA screening test is the only way to find prostate cancer (unless a digital rectal exam is performed or the cancer is found performing CtScan or MRI for another reason) before it spreads to other organs (metastasizes) and becomes very hard to treat.
Prostate cancer has a good prognosis because most prostate cancers are dormant. If a cancerous tumor is found, it is impossible to tell if the tumor will become active or be dormant for the rest of your life. Treatment for prostate cancer has some significant risks including impotence. Therefore, the trend in medicine is to watch and wait (active surveillance using repeated PSA and/or MRIs to ensure the tumor has not grown), intervening down the road only if the cancer becomes active.
One in seven men will be diagnosed with prostate cancer in their lifetime, but few will die of it. It is the fifth leading cause of death by cancer in men, but it is so slow growing that the survival rate is nearly 100% five years after diagnosis.
If you are healthy, with no symptoms of prostate cancer and don’t fall into the high risk group, and are considering having a PSA screening test, you should carefully consider the choices you will have if a high PSA score comes back (indicating the possibility of prostate cancer). An informed discussion with your physician explaining risks, side effects and benefits is essential. This test only gives a higher chance of survival for men who are at high risk of prostate cancer.
Pros | Cons | What to Do
The PSA (prostate-specific antigen) test measures the protein produced by normal as well as malignant cells in the prostate gland. Even if you have a normal prostate, you will have some of that protein in the blood. The results are interpreted by a specialist as high (positive) or low (negative). PSA results should be interpreted differently based on age, race, medication interactions and other factors.
But the PSA test for prostate cancer is controversial because PSA levels are affected by many factors other than prostate cancer — and that leads to a high number of false positives for prostate cancer. A study published in the New England Journal of Medicine in 2009 stated, “The rate of overdiagnosis of prostate cancer (defined as the diagnosis in men who would not have clinical symptoms during their lifetime) has been estimated to be as high as 50% in the screening group.”
Because of that finding, the American Cancer Society and the USPSTF (US Preventive Services Task Force) do not recommend screening men routinely. The American Urological Society does recommend the test within certain parameters.
However, some doctors still use the PSA test as a screen on otherwise healthy, non-symptomatic men. Your informed decision to screen or not should be based on your preference after consultation with your doctor.
Since prostate cancer is so common and so deadly, why don’t all men get screened? Read on and watch MedShadow TV for a short overview.
The Pros of the PSA Screening Test
It could save your life. The PSA test for prostate cancer is the only way to find this cancer before it becomes metastatic, meaning before it has spread to other organs. Without the screening test, it is very unlikely that it will be caught early because many of the cancers of the prostate have no symptoms. Catching aggressive prostate cancer early, before it is metastatic, is crucial to survival.
Cons — Against Screening
PSA tests for prostate cancer don’t really tell you if you have that cancer. False positives are when the screening or test results in a “high reading” of PSA. Just like with breast cancer mammograms, a positive test can’t be trusted; instead, it is the starting point of further testing or watchful waiting.
PSA tests have been estimated to have about a 25% false positive rate, depending on the doctor’s PSA cut-off number. A false positive leads to unnecessary further testing (that can cause harm to you, not to mention time and cost) and a lot of stress.
Many things can cause a high reading — a false positive. Known issues such as prostate hyperplasia or prostatitis, a recent rectal exam, a UTI (urinary tract infection) and even a lot of sex can falsely increase the PSA reading!
False negatives or false low readings
A false low reading will indicate no cancer when there is. Using statins, NSAIDs (nonsteroidal anti-inflammatory drugs) such as Tylenol (acetaminophen) and Advil (ibuprofen) and diuretics can lower the PSA reading. Proscar and Propecia (both finasteride), whether used for an enlarged prostate or hair loss, can lower the reading.
The PSA test by itself can only indicate the possibility of cancer.
The test cannot indicate the difference between a slow-growing cancer and an aggressive cancer. It cannot determine the stage. After going through more tests, the PSA test for prostate cancer is used as a part of the pretreatment staging (see below for staging).
Overtreatment risks
Being treated for cancer unnecessarily because of a false positive exposes men to the risk of side effects with no benefit — that is overtreatment. Treating a man over the age of 75 for prostate cancer is usually overtreatment because prostate cancer is slow growing and that man will likely die of other causes before the prostate cancer becomes life threatening.
Overtreatment is harmful because the side effects of prostate cancer treatment are impotence, incontinence and infection, among others, not to mention stress. Not everyone will get any or all side effects, but some will.
So there you have it — a screening test that could either save your life or ruin your quality of life unnecessarily.
The Takeaway
Don’t take the PSA test if you are over 75 because it is a slow-growing cancer and you’ll likely die of something else.
If you are between the ages of 50 and 74, talk to your doctor. African-American men and others in the high-risk category should start at 45 years old with a frank discussion of what your personal risks are and what actions you would be willing to take if a high reading came back, so you’ll be able to make an informed opinion. Here is an interesting essay written by a doctor with prostate cancer, Prostate Cancer and the Waiting Game.
I certainly would not suggest that you take the PSA screening test regularly if you are under 50 unless you have a high risk. What is high risk? A family history of prostate cancer, the BRCA1 or BRCA2 genetic mutation (the same mutation as breast cancer, among other cancers) or you are African-American. It’s not known why, but the African-American population has a higher risk of prostate cancer.
A large, new study was just published in JAMA which had interesting but probably not very useful results. The study reported on more than 400,000 men aged 50 – 69 years. About 36% were given the PSA test. The entire group was followed for 10 years. Some of the men in both the PSA-tested group and those who did not did get the test did get prostate cancer during the decade of the study. However the number of men who died of prostate cancer was about the same in the 2 groups. Prostate cancer takes a long time to grow so following these men for another 5 or 10 years might yield a different result. Conclusion? Having only a single test is not helpful. A rising PSA value — based on 2 or more tests — is the better predictor.
As a doctor, I would recommend a series of the PSA screenings for men between the ages of 50 and 75, if you are comfortable with the risks of possible over-treatment. Remember, the PSA test gives the doctor a reading of the protein produced by the prostate gland, whether normal or malignant.
What to Do If You Receive a High PSA Reading?
A high reading can be different from person to person and depends both on your age (which is why many doctors suggest a baseline before the age of 50) and the change over time (escalation velocity) of the rise in number. In general, men under the age of 60 are expected to have a PSA reading below 2.5 and men over 60 a reading of under 4.0.
If you take the test and get back a high reading, the most important thing is to manage the results in an intelligent way. A positive PSA test is just the beginning.
Once identified, cancer has to be tracked, biopsied, staged and treated. It is impossible to tell if the cancer is the fast-growing type or the indolent, slow-growing, so all prostate cancers are treated as if they are deadly. That means that many people who have an indolent form of cancer will be over-treated, which has many consequences. Don’t hurry into treatment. Take the time to make an informed decision.
1. Confirm or rule out cancer
- You should be referred to a urologist immediately.
- Then do nothing. As difficult as it seems, it is almost always recommended to wait 2 months and take the PSA test again (active surveillance).
- If the PSA results are rising (meaning that they change over time even if they stay in the normal range), your doctor will likely suggest a digital rectal exam, which is low risk and not invasive like a biopsy. The doctor will be attempting to find a tumor by touch. Not every tumor can be felt by a doctor, either because it is too small or it’s in an area the doctor cannot reach. For that reason, the digital rectal exam might confirm a tumor, but it cannot rule out cancer.
- A TRUS (transrectal ultrasound) will give your doctor much more information on whether there is a tumor, its size and location.
- Before the procedure, your doctor will discuss the risks and benefits of conducting a needle biopsy during the TRUS. A biopsy confirms if it is cancer or not. If cancer, the biopsy results are key to getting an accurate staging before treatment. Generally biopsies are considered safe, with a small risk of infection or other complications. However, other health issues such as diabetes can add complication possibilities.
- The multiparametric MRI (a type of 3-dimensional MRI), which explores the area of the tumor for diagnosis, can be used as an additional diagnostic tool. Some insurance companies may not cover this process.
2. If the biopsy confirms cancer, further evaluation is crucial for best treatment options
The evaluation includes pretreatment staging in 3 parts:
-
- The clinical staging encompasses 3 categories named T, N and M. Each of the letters will be assigned either an “x,” which means not determined, or a number from 0-4 (4 is more advanced).
• T category indicates the extent of the main tumor.
• N category indicates if the cancer has yet spread to the lymph nodes.
• M category indicates if the cancer has metastasized to other parts of the body.
- 2. Histopathology staging is based on the sum of the Gleason scores. A Gleason score is derived from 2 examinations of the biopsy — the first evaluating the architectural features of the prostate gland, and the second looking at the level of abnormality of the cell nucleoli. The combined total is the Gleason score.
- 3. The PSA level at time of diagnosis (not from the first PSA reading).
Other tests can be used in developing the treatment plan. Multiparametric MRIs are becoming more commonly included in the staging, and CT bone scans are sometimes used for more-detailed staging, particularly when the Gleason score is over 7 and/or if the PSA is over 10.
A chart describing what the specific TNM scores mean in staging of prostate cancer can be found at Cancer.org
At this point you and your doctors will determine a personal plan for your care.
— With Suzanne B. Robotti