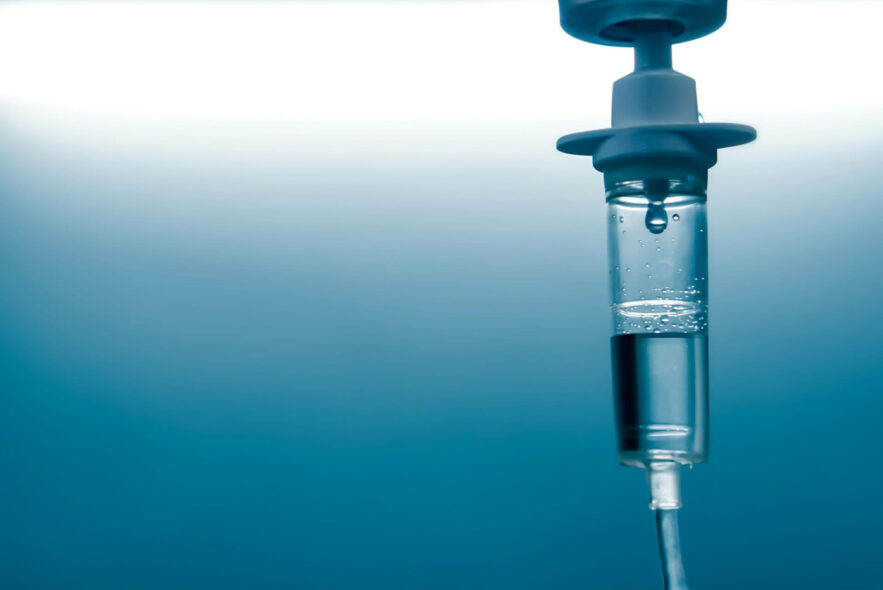
One of the defining characteristics of cancer is the speed at which the cells divide (multiply). Chemotherapy targets quickly dividing cells which it is why it can be effective in shrinking cancer tumors. But chemo travels throughout your body and is non-selective, meaning the drugs kill any cell that divides quickly anywhere in your body. Because of that, chemo has limited effectiveness and, as is widely known, very bad side effects. Is Artificial Intelligence the answer?
Synthetically Lethal Interactions
One targeted approach to cancer therapy is to exploit the unique mutations of cancer cells (many cells have mutations, there are millions of mutations). The idea is if a scientist can identify a unique mutation in the particular cancer tumor then the scientist can find a second mutation that is harmless to healthy cells – but selectively kills the cell that carries the cancer mutation. Then a chemo formula can be developed to send that second mutation affecting every cell in your body – but it will only kill the cancer cells that have the first mutation. The concept is complicated, involving proteins and inhibitors and is called “synthetically lethal interactions.” It’s described more fully in this paper from the National Institutes of Health, Harnessing synthetic lethal interactions in anticancer drug discovery.
Problem is, finding that second mutation to pair with the first mutation is incredibly time consuming. A research paper published in the journal PLOS:Computational Biology reported on a new algorithm called “SLant,” (Synthetic Lethal analysis via Network topology) that predicts lethal pairs. SLant was created by Researchers at the University of Sussex and the Institute of Cancer Research in London and is now available in a database called “Slorth” (SL – Synthetic lethality, ORTH – orthology data. I don’t name these things, I just report on them).
One of the authors of the study, Dr. Frances Pearl, Director of Doctoral Studies, School of Life Sciences, University of Sussex, England, told MedShadow that the process of synthetic lethality is in limited use now. “PARP inhibitors (eg olaparib) are licensed for use in BRCA1 or BRCA2 deficient cancers (breast and ovarian are licensed, pancreatic cancers in clinical trial). Our database presents our predictions and reports in vitro experiments. Far more target validation would be required before using results clinically.”
The expectation is the ability to develop chemo formulae to target only the cancerous cells in a specific tumor should make chemo more effective, less destructive to the rest of your body and result in fewer side effects.