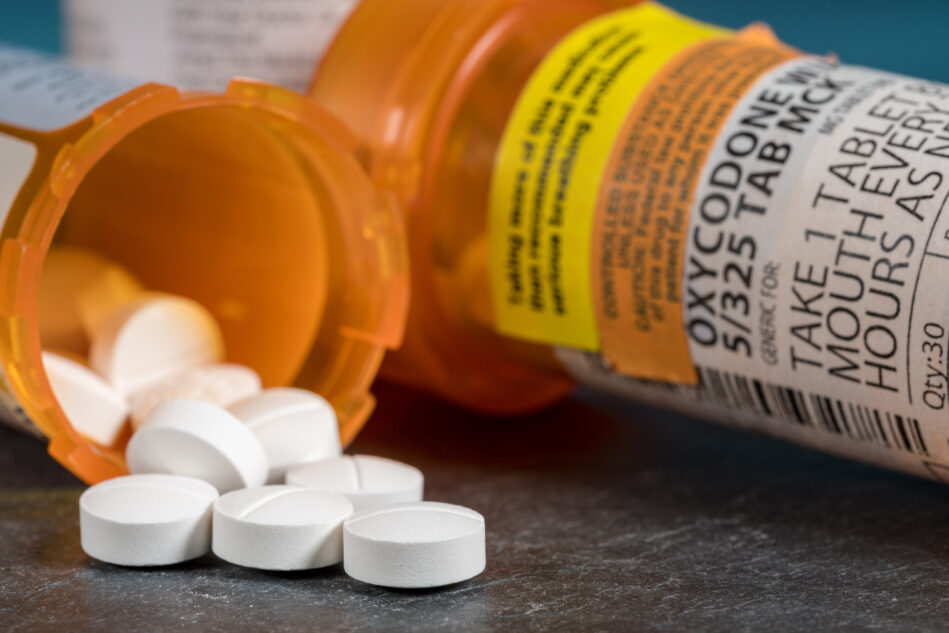
The US is in the throes of a drug overdose crisis. “Morphine [an opiate] and other prescription-painkiller abuse is more of a problem than heroin or any street drug,” hospital pharmacist Ray Murphy said seven years ago.
“The prescribers are part of the problem. Some doctors don’t investigate their own patients enough before refilling a prescription,” he said, adding that if a patient is requesting that a opioid prescription be refilled, it’s possible the patient now needs morphine to support a habit. In that case, the doctor might consider treatment for an opioid-use disorder (OUD).
“Morphine can be a wonderful drug for pain relief, if you break a bone, have a heart attack or have pain after surgery,” said Norman Wetterau, MD, public policy committee chair of the New York Society of Addiction Medicine. “But people get into trouble when it is used for chronic pain.”
In the early 2010s, prescription drug monitoring programs (PDMPs) were widespread. Now doctors in every state, except Missouri, can review their patient’s prescription history and make more informed decisions about how to prescribe opioids. In some states, physicians are required to do so. This, and other new regulations have led some patients who suffer from chronic pain to argue that necessary medicines are being withheld from them.
But while opioid use disorders may be a risk of prescription painkillers, today 85% of overdoses — the most serious consequence of OUDs — include at least one illicitly manufactured drug like heroin, methamphetamine or fentanyl created outside of pharmaceutical labs, rather than just prescription drugs like morphine.
Why People Develop Opioid-Use Disorders (OUDs)
Misuse of prescription painkillers, including morphine, was the second most common form of illicit drug use, after marijuana, in 2018, according to the Substance Abuse and Mental Health Services Administration’s “National Survey on Drug Use and Health.” Nearly 8% of people who took morphine that year misused the drug, meaning they acquired it without their own prescription, or took it in greater amounts or more often or for longer periods than directed by a doctor. More than half of those users bought, stole or were given the drug by a friend or relative.
A person develops an OUD for a variety of reasons. Substance-use disorders are frequently comorbid with conditions like anxiety, depression and PTSD (post-traumatic stress disorder); nearly two-thirds of people diagnosed with an OUD also have or have had a mental illness.
Last year, there was a jump in opioid overdoses, attributed to the COVID-19 pandemic. Experts suggest that the social distancing required to help contain the virus’s spread led to isolation and despair, both of which are risk factors for substance use disorders.
In Kentucky, researchers compared the number of emergency medical services (EMS) runs responding to an opioid overdose in the 52 days before and after the COVID-19 emergency declaration on March 6, 2020. After the declaration, the number of overdose runs, in which patients needed transport to a hospital increased by 17%,; and there was a 71% rise in patients who refused a ride to a hospital; suspected overdose deaths rose by 50%. During that same period, EMS runs for other conditions declined or leveled off.
Similarly, in an emergency department at a Virginia hospital, prescription painkiller overdose visits more than doubled, from 102 between March and June 2019, to 227 between March and June in the next year, according to a study from the Virginia Commonwealth University.
The Signs of OUDs and Overdoses
The side effects of morphine use, misuse and the symptoms of opioid withdrawal paint an unsettling picture. In short, this potent opioid can bring on addiction, overdose and death. Depending on the individual and the dose taken, typical side effects are nausea, vomiting, stomach pain, constipation, dizziness, drowsiness, headache and feelings of apathy or anxiety. Infrequent side effects range from dry mouth to sexual dysfunction. On the list of rare, but severe, side effects are seizures, shock, hallucinations, chest pain, circulatory problems and intestinal blockage. However, “respiratory depression is the most worrisome side effect of all,” because it can lead to lung failure, coma and death, said Damon Raskin, MD, an internist and addiction medicine specialist in Pacific Palisades, California. Symptoms such as constipation or drowsiness may not warrant a visit to the ER, but you should still talk them over with your doctor “However, the other severe symptoms are cause for alarm,” Raskin explains, emphasizing the need for immediate treatment.
How Does Morphine Work?
Morphine is in the opiate class of drugs delivered by injection, liquid, tablet or capsule. German pharmacist Friedrich Serturner created morphine in the early 1800’s. The drug is derived from opium, found in the unripened seedpods of the Asian poppy plant.
Morphine attaches to opioid receptors in the brain and throughout the central nervous system and blocks the perception of pain. Because morphine was so effective in relieving pain, it quickly became popular. By the mid-19th century, its use was widespread in the US, especially for injured soldiers.
Morphine brand names include Apokyn, Duramorph, Infumorph, Kadian, Kynmobi, Mitigo and MS Contin. Morphine’s potentially dangerous effects are well-documented. Gregory Skipper, MD, medical director of the Center for Professional Recovery at the luxury rehabilitation facility Seasons in Malibu, California, warns, “Any drug that stimulates the opioid receptors is going to be addictive.”
The Trend of Liberal Prescribing
A study from the George Washington School of Medicine & Health Sciences found that the percentage of US ER visits in which an opioid was prescribed increased by a third in a nine-year period, from nearly 21% in 2001 to 31% in 2010. However, this trend leveled off and reversed through 2017, according to the latest statistics reported by the Centers for Disease Control and Prevention (CDC). Between the study’s periods 2006 to 2007 and 2016 to 2017, the CDC reports a 23% drop in opioid prescriptions given to patients when they were discharged from the ER. The researchers suggest that implementation of drug-monitoring programs along with federal, state and local programs aimed at changing prescribing practices have contributed to the decrease in opioid prescriptions.
In spite of the decline in ER prescription painkiller prescribing, the CDC reports that the morphine milligram equivalents (MMEs) — the strength of the opioid dosage based on the equivalent number of milligrams of morphine — prescribed per person in the US are three times what they were in 1999. The MME provides a means of comparing the strength of different opioid drugs and gauges the overdose potential of an opioid dose.
According to the Physicians for Responsible Opioid Prescribing (PROP), the practice of long-term opioid therapy for noncancer patients has grown significantly in the last 30 years in tandem with a corresponding rise in addiction, overdose and fatalities.
Before that, morphine was typically prescribed for a limited number of patients, including those in hospice and for palliative care, for cancer and postoperative pain, and for heart attack and traumatic injuries commonly seen in the ER. In recent years, morphine prescribing has expanded to include a long list of other ailments, such as pancreatitis, kidney stones, appendicitis, fibromyalgia, chronic back pain and headache.
Jane C. Ballantyne, MD, PROP’s president, attributed some of the increased prescribing of morphine to “aggressive marketing by the pharmaceutical industry.”
Indeed, a 2019 study from the University of Pittsburgh suggests that drug company gifts to prescribers may have increased the amount of opioids being prescribed. The researchers examined two years of prescribing data from 236,103 physicians who accepted gifts from pharmaceutical firms and prescribed opioids the following year. Primary-care physicians who received such gifts valued at $100 or more were 3.5 times more likely to be the highest prescribers of opioids in their specialty in the year after they received them. Psychiatrists and neurologists who accepted $100 or more in gifts were up to 13 times more likely to be the highest opioid prescribers compared to their colleagues.
If you want to know if your doctor accepts payments or gifts from pharma firms, ProPublica publishes reports in its easily searchable database, called Dollars for Docs. Doctors are now required by law to report all gifts and payments from drug companies.
The World Health Organization’s (WHO) guidelines for pain intervention state that morphine administration be limited strictly to treat moderate and severe pain. The risk-benefit scale slides into dicey territory when a patient has chronic, long-term opioid therapy, notes Anna Lembke, MD, medical director of addiction medicine at Stanford University. “It’s important to realize that opioids are not actually effective for all chronic pain and can, in some instances, even make pain worse by causing a condition called ‘opioid-induced hyperalgesia.’ ” This is a phenomenon whereby long-term use of morphine and other opioids can cease to manage pain and sometimes cause pain, while upping physical dependence. At this point, use of the drug should most likely be tapered off.
In the Emergency Room
Morphine treatment is most beneficial for blunting acute pain caused by trauma and serious disease. A severe heart attack, burns and broken bones fit very well into this criteria. However, if someone comes to the ER with a minor injury, “it might be appropriate to treat them with other analgesics or local anesthetics, or no pain meds at all,” said Ballantyne. She asserts that no patient should walk out of the ER with more than two morphine pills in hand.
Jayaram Srinivasan Brindala, MD, a preventive medicine specialist in Maitland, Florida, said, “Effective non-opioid pharmacological treatment of pain may include numerous options, such as aspirin, acetaminophen, nonsteroidal anti-inflammatory drugs (NSAIDs), anticonvulsants, tricyclics, serotonin-norepinephrine reuptake inhibitors (SNRIs), antispasmodics, topical analgesic agents and others.”
In Palliative and Hospice Care
According to the National Institute on Aging (NIA), morphine use in palliative care can successfully reduce pain and shortness of breath. For patients with COPD (chronic obstructive pulmonary disease), heart failure or Parkinson’s disease, the benefits from carefully measured morphine therapy can improve the quality of life with whatever time remains.
“I believe that good pain relief can help a patient want to live, say goodbye to their family and complete other unfinished tasks,” said Wetterau. “If the dose of morphine is increased too rapidly, it could hasten death by decreasing or stopping respiration.”
While morphine does slow the body’s systems, the NIA notes that if dosages are increased judiciously, most experts believe that taking morphine for palliative care at the end of life is unlikely to speed death.
Factors to Consider
The risk-benefit analysis of prescription painkiller dosing is a complex subject with no simple answers. There are drug and disease interactions that should be carefully weighed before a person agrees to a course of morphine treatment. If you have liver or kidney disease, a traumatic brain injury, severe asthma or COPD, a sluggish gastrointestinal system or a history of substance-use disorder, you may not be a good candidate for non-palliative morphine therapy.
According to Drugs.com, as of December 2020, of the 416 potential drug interactions with morphine, 118 are of major concern. One of them, monoamine oxidase inhibitors (MAOIs ) can result in serious side effects, including a coma, excitability, low blood pressure, shallow or slowed breathing, shaking or twitching and more. Drugs in this classification, including phenelzine (Nardil), tranylcypromine (Parnate), isocarboxazid (Marplan) or selegiline (Zelapar), should be discontinued at least 14 days before starting a course of morphine pain management. Once morphine therapy begins, the patient must be monitored carefully. When is morphine safe to use? “It’s never safe, not completely… it’s a dangerous drug,“ said Ballantyne. She maintains that a maximum course of three days will satisfy even acute-pain-intervention needs.
Alternative Pain Interventions
In its “Guidelines for Prescribing Opioids for Chronic Pain,” the CDC recommends nonpharmacologic treatments, such as cognitive behavioral therapy (CBT) and exercise therapy, before trying opioids. In CBT, a therapist works with patients to help replace negative self-destructive ways of thinking with more realistic, positive thoughts.
A study published in the European Journal of Physical and Rehabilitation Medicine found that a program of four CBT sessions followed by 10 sessions of exercise training reduced disability and improved quality of life in those with chronic neck pain. Key to the program’s success was reduction in participants’ “kinesiophobia,” an irrational fear of movement over concern of injuring oneself again.
Research has also shown that mindfulness meditation provides multiple benefits in dealing with chronic pain, as well as some relief from and improvement in quality of life. In a University of Pittsburgh study published in JAMA Internal Medicine, researchers tested mindfulness meditation in a group of adults aged 65 and over with chronic low-back pain. Half the group received eight weeks of mindfulness meditation training. The other half participated in an education program on healthy aging. At the end of the eight-week period, participants who practiced mindfulness meditation experienced significant reduction in current pain, peak pain intensity in the past week and improved physical function compared to those who participated in the education program.
A program known as mindfulness-oriented recovery enhancement (MORE) has shown promise in helping people with chronic pain on long-term opioid treatment reduce their opioid intake. MORE sessions provide instruction in mindfulness and techniques to increase self-control and emotion regulation and to savor pleasant events and emotions.
In one study, patients reduced their opioid dosing by 32% after eight weeks of MORE training compared to those in a support group. A 2019 study published in the journal Drug and Alcohol Dependence tested MORE in people with chronic pain who had an opioid-use disorder and were on methadone-maintenance therapy. After eight two-hour sessions, those who participated in MORE reported reduced intensity of opioid craving, pain unpleasantness and stress. Researchers suggest that MORE boosts self-regulation and facilitates self-control over opioid use, enabling those in chronic pain to reduce their use of opioids.
Ivy Branin, a naturopathic doctor in New York City, believes in “getting to the source of the pain first and using the least invasive approach to pain management.” She advocates dietary intervention for inflammation, which is often the cause of pain. For example, eliminating refined carbohydrates and red meat and ramping up omega-3 fatty acids can reduce inflammation. She also recommended other natural-healing modalities to target pain, such as acupuncture, biofeedback, chiropractic treatment and yoga.
Over time, proactive steps of patients and doctors can help curb the excessive use of opioids in the US. The medical community needs better education for its pain-intervention protocols, and patients need a supportive network for pain-management advocacy. The final consensus is that active engagement in multiple pain-management modalities is likely to achieve the best outcomes.