Article HTML
<!-- wp:paragraph -->
<p><a href="https://www.cdc.gov/bloodpressure/about.htm" target="_blank" rel="noreferrer noopener">High blood pressure </a>(hypertension) is sometimes called the “silent killer.” It often has no symptoms at all, but it can raise your risk of deadly events such as heart attacks and strokes while slowly damaging your organs over time.<sup>1</sup> How high exactly are these risks, and what can you do about high blood pressure? Here’s what to know about hypertension. </p>
<!-- /wp:paragraph -->
<!-- wp:heading -->
<h2 class="wp-block-heading" id="h.etc2ovnbjn7y">What Do the Top and Bottom Numbers Mean on Your Blood Pressure Reading?</h2>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Blood pressure<sup>1</sup> is the amount of pressure that your blood exerts against your blood vessels. Systolic pressure is the top number. That represents the pressure when your heart contracts and pushes your blood out to your organs. The bottom number is diastolic blood pressure, the pressure when your heart relaxes and is filling up. They’re both measured in millimeters of mercury (mm Hg), a unit of pressure. While both numbers are important, systolic pressure is the one that healthcare providers usually focus on for most people.</p>
<!-- /wp:paragraph -->
<!-- wp:heading -->
<h2 class="wp-block-heading" id="h.4nd6yhi528fd">What’s a Normal, Healthy Blood Pressure?</h2>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Most organizations recognize that there is “normal” or healthy blood pressure, elevated blood pressure, and hypertension. If your blood pressure falls in the elevated range, you are at risk for developing hypertension. The American Heart Association defines elevated blood pressure in adults as starting at 120 mm Hg/80 mm Hg and hypertension as beginning at 130 mm Hg/ 80 mm Hg. If your blood pressure is high on one reading, you’ll need to have it measured a second time on a separate day to confirm the accuracy of the reading. Your healthcare provider may suggest getting a blood pressure cuff to use on your own at home, to rule out the possibility that your readings are only high in the doctor’s office but normal at home.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Previous guidelines from 2003 considered the cutoffs for elevated blood pressure and hypertension to be 130mmHg/80mmHg and 140 mmHg/80 mmHg, respectively.<sup>1</sup> <a href="https://www.facebook.com/sharer/sharer.php?u=https%3A%2F%2Fmedshadow.org%2Feverything-you-need-to-know-about-blood-pressure-2%2F" target="_blank" rel="noreferrer noopener"></a></p>
<!-- /wp:paragraph -->
<!-- wp:html -->
<script src="https://static-bundles.visme.co/visme-embed.js"></script>
<div class="visme_d" data-title="BP Meter w/ label" data-url="01eo74y6-bp-meter-w-label" data-w="816" data-full-h="true" data-h="1056" data-domain="my"></div>
<!-- /wp:html -->
<!-- wp:paragraph -->
<p></p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>If your physician says you have high blood pressure, you should ask how high it is and what that means about your risk for cardiovascular events. In some cases, if your blood pressure is very high, you’ll need medication right away to get your blood pressure under control. If it’s only a little bit elevated, it is recommended to try lowering it through <a href="https://medshadow.org/hypertension-blood-pressure-lower/" target="_blank" rel="noreferrer noopener">lifestyle changes</a> before trying medication.</p>
<!-- /wp:paragraph -->
<!-- wp:heading -->
<h2 class="wp-block-heading" id="h.qsgx4f5x58h9">Sex Differences in Blood Pressure</h2>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Men and women have different baseline blood pressures and <a href="https://www.ahajournals.org/doi/10.1161/CIRCULATIONAHA.120.049360" target="_blank" rel="noreferrer noopener">r</a><a href="https://www.ahajournals.org/doi/10.1161/CIRCULATIONAHA.120.049360" target="_blank" rel="noreferrer noopener">ecent research</a><sup>2</sup> also suggests that women may be better off keeping their blood pressure even lower than their male counterparts, though this hasn’t translated into unique guidelines yet. In the study of 27,452 participants, the women started experiencing a higher risk of cardiovascular disease and events like heart attacks and strokes at lower systolic blood pressures than the men.</p>
<!-- /wp:paragraph -->
<!-- wp:html -->
<script src="https://static-bundles.visme.co/visme-embed.js"></script>
<div class="visme_d" data-title="Hypertension prevalence, by gender" data-url="eprvjo6r-hypertension-prevalence-by-gender-2" data-w="100%" data-full-h="true" data-h="100%" data-domain="my"></div>
<!-- /wp:html -->
<!-- wp:heading -->
<h2 class="wp-block-heading" id="h.32mre6fftad2">Symptoms of High Blood Pressure</h2>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Typically you won’t have any symptoms of hypertension. The only way to know if you have it is to measure your blood pressure.</p>
<!-- /wp:paragraph -->
<!-- wp:heading -->
<h2 class="wp-block-heading" id="h.m2x9os2p931j">When is High Blood Pressure an Emergency?</h2>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>While any elevated blood pressure is worth discussing with your doctor, if your blood pressure reads higher than 180 mm Hg/120 mm Hg, you should wait five minutes and take it again, according to the <a href="https://www.heart.org/en/health-topics/high-blood-pressure/understanding-blood-pressure-readings/hypertensive-crisis-when-you-should-call-911-for-high-blood-pressure" target="_blank" rel="noreferrer noopener">American Heart Association</a>.<sup>3</sup> If it remains elevated, you could be experiencing hypertensive urgency or a hypertensive emergency.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>If your <a href="https://www.who.int/news-room/fact-sheets/detail/hypertension" target="_blank" rel="noreferrer noopener">blood pressure is extremely high</a><sup>4</sup> (more than 180 mm Hg/120 mm Hg, for example) you might have a severe headache, chest pain, vomiting, confusion, fainting, shortness of breath, a nosebleed, ringing or buzzing in your ears, an abnormal heart rhythm or difficulty breathing. If you have any of these symptoms, especially with a high blood pressure reading, you should go to the emergency room.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>If your blood pressure is above 180 mm Hg/120 mm Hg and you don’t feel any other symptoms, it’s considered hypertensive urgency. You should call your cardiologist or healthcare provider right away.</p>
<!-- /wp:paragraph -->
<!-- wp:heading -->
<h2 class="wp-block-heading" id="h.i8os6lmy47j2">Hypertension Prevalence by Ethnicity</h2>
<!-- /wp:heading -->
<!-- wp:html -->
<script src="https://static-bundles.visme.co/visme-embed.js"></script>
<div class="visme_d" data-title="US adults with hypertension, by ethnicity" data-url="z4rmjjj1-us-adults-with-hypertension-by-ethnicity" data-w="100%" data-full-h="true" data-h="100%" data-domain="my"></div>
<!-- /wp:html -->
<!-- wp:paragraph -->
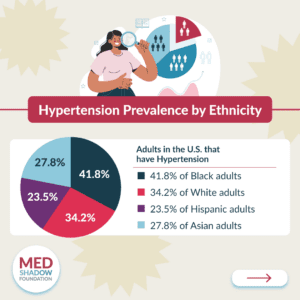
<p>Out of the entire adult population in the United States, 33% of adults had a diagnosis of hypertension according to an <a href="https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10861176/" target="_blank" rel="noreferrer noopener">analysis of three National Health and Nutrition Examination Survey (NHANES) studies</a><sup>5</sup> conducted between 2013 and 2018, but the prevalence differed based on ethnicity.</p>
<!-- /wp:paragraph -->
<!-- wp:image {"id":831,"sizeSlug":"full","linkDestination":"none","align":"left"} -->
<figure class="wp-block-image alignleft size-full"><img src="https://medshadow.org/wp-content/uploads/2024/05/etny-300x300-1.png" alt="" class="wp-image-831"/><figcaption class="wp-element-caption">Hypertension Prevalence</figcaption></figure>
<!-- /wp:image -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>41.8% of Black adults in the U.S. were found to have hypertension.</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>34.2% of white adults in the U.S. were found to have hypertension.</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>23.5% of Hispanic adults in the U.S. were found to have hypertension.</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>27.8% of Asian adults in the U.S. were found to have hypertension.</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>32.0% of Americans of other ethnicities were found to have hypertension.</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:paragraph -->
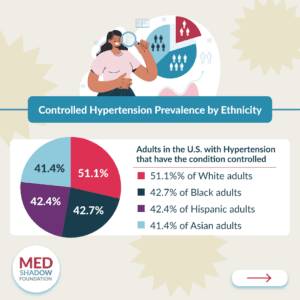
<p>Only 48.6% of adults with hypertension in the U.S. had the condition well-controlled. The researchers defined “well-controlled” as blood pressure that was under 140 mm Hg/90 mm Hg.</p>
<!-- /wp:paragraph -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>51.1% of white adults in the U.S. with hypertension had the condition controlled.</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>42.7% of Black adults in the U.S. with hypertension had the condition controlled.</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>42.4% of Hispanic adults in the U.S. with hypertension had the condition controlled.</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>41.4% of Asian adults in the U.S. with hypertension had the condition controlled.</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>52.0% of Americans of other ethnicities with hypertension had the condition controlled.</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:image {"id":832,"sizeSlug":"full","linkDestination":"none","align":"right"} -->
<figure class="wp-block-image alignright size-full"><img src="https://medshadow.org/wp-content/uploads/2024/05/etn2-300x300-1.png" alt="" class="wp-image-832"/><figcaption class="wp-element-caption">Hypertension Prevalence<br></figcaption></figure>
<!-- /wp:image -->
<!-- wp:paragraph -->
<p>It’s important to note that these differences in prevalence and blood pressure control are primarily due to <a href="https://www.heart.org/en/health-topics/high-blood-pressure/why-high-blood-pressure-is-a-silent-killer/high-blood-pressure-and-african-americans" target="_blank" rel="noreferrer noopener">social determinants of health</a>—differences in access to healthy foods, green spaces, and high-quality healthcare, among other things. </p>
<!-- /wp:paragraph -->
<!-- wp:html -->
<script src="https://static-bundles.visme.co/visme-embed.js"></script>
<div class="visme_d" data-title="Prevalence of hypertension" data-url="pvm0y0y4-prevalence-of-hypertension" data-w="100%" data-full-h="true" data-h="100%" data-domain="my"></div>
<!-- /wp:html -->
<!-- wp:heading -->
<h2 class="wp-block-heading" id="h.2qiij1h0uv3x">Hypertension in Pregnancy</h2>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Many women have hypertension and need to manage their condition throughout a pregnancy, but sometimes it’s diagnosed for the first time at this point in a woman’s life. In many cases, hypertension that’s diagnosed during pregnancy is associated with a dangerous, but relatively common, condition called <a href="https://medshadow.org/preeclampsia-what-you-need-to-know/" target="_blank" rel="noreferrer noopener">preeclampsia</a>.</p>
<!-- /wp:paragraph -->
<!-- wp:heading -->
<h2 class="wp-block-heading" id="h.x58o0n78yvtj">Causes of High Blood Pressure</h2>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>There are many causes of high blood pressure. Primary hypertension is hypertension without a known cause. Secondary hypertension is due to another underlying condition. Researchers have found that it’s <a href="https://www.ahajournals.org/doi/10.1161/circresaha.116.305697" target="_blank" rel="noreferrer noopener">more common</a><sup>6</sup> in people who carry extra weight or have <a href="https://medshadow.org/obesity-causes-risks-treatment-options-and-side-effects/" target="_blank" rel="noreferrer noopener">obesity</a>. It’s also common in people with hormonal disorders such as women with <a href="https://medshadow.org/pcos-treatment-management-and-medications/" target="_blank" rel="noreferrer noopener">polycystic ovary syndrome (PCOS)</a>, kidney disease, obstructive sleep apnea, or other cardiovascular conditions. High blood pressure can also be a <a href="https://medshadow.org/blood-pressure-changes-side-effect/" target="_blank" rel="noreferrer noopener">side effect of medications</a> for a variety of conditions.</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":3} -->
<h3 class="wp-block-heading" id="h.chl5bt60vups">Could My High Blood Pressure Be a Side Effect?</h3>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Many drugs can raise or lower blood pressure as a side effect. Some medications known to raise blood pressure are:</p>
<!-- /wp:paragraph -->
<!-- wp:image {"id":833,"sizeSlug":"full","linkDestination":"none","align":"left"} -->
<figure class="wp-block-image alignleft size-full"><img src="https://medshadow.org/wp-content/uploads/2024/05/medications-300x300-1.png" alt="" class="wp-image-833"/><figcaption class="wp-element-caption">Medications can cause hypertension<br></figcaption></figure>
<!-- /wp:image -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>Decongestants</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Caffeine</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Corticosteroids</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Nonsteroidal anti-inflammatory drugs (NSAIDS)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li><a href="https://www.aafp.org/afp/2007/0415/p1252.html#:~:text=Studies%20have%20shown%20that%20the%20use%20of%20oral%20contraceptives%20(including,and%206%20mm%20Hg%20diastolic." target="_blank" rel="noreferrer noopener">Oral contraceptives</a></li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Serotonin norepinephrine reuptake inhibitors (SNRIs)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Atypical antipsychotics</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Amphetamines</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Immunosuppressants</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Recreational drugs</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:paragraph -->
<p>Nearly 15% of adults in the U.S. reported taking drugs that could be raising their blood pressure, according to a <a href="https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2786014" target="_blank" rel="noreferrer noopener">2021 study in JAMA.</a><sup>7</sup></p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Read more about how common drugs can influence your blood pressure in <em>MedShadow’s</em> <a href="https://medshadow.org/blood-pressure-changes-side-effect/" target="_blank" rel="noreferrer noopener">Are Changes in Blood Pressure a Side Effect of Your Medication?</a></p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":4} -->
<h4 class="wp-block-heading" id="h.pq9bfg2rm8vv">Does Testosterone Raise Blood Pressure?</h4>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>There’s <a href="https://medlineplus.gov/druginfo/meds/a619028.html#:~:text=Testosterone%20may%20cause%20an%20increase,heart%20attack%2C%20or%20a%20stroke." target="_blank" rel="noreferrer noopener">some evidence</a><sup>8</sup> that taking testosterone replacement therapy can raise blood pressure in men. However, a 2023 study <a href="https://medshadow.org/should-i-try-to-boost-my-testosterone-levels/#Long-Term_Effects_of_HRT_for_Men" target="_blank" rel="noreferrer noopener">complicated the picture</a>.<sup>9</sup> It showed that men who were prescribed testosterone replacement therapy to treat low levels of the hormone didn’t have any more heart attacks or strokes (which are dangers associated with high blood pressure) over the course of two years than men who took placebo. The men who took testosterone did have more instances of pulmonary embolism, acute kidney injury, and irregular heart rhythms though.</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":3} -->
<h3 class="wp-block-heading" id="h.l6qcgh6tlxme">Does Alcohol Raise Blood Pressure?</h3>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Even just one drink a day may slightly elevate your blood pressure over time, according to a 2023 meta-analysis published in the journal, <em><a href="https://www.ahajournals.org/doi/10.1161/HYPERTENSIONAHA.123.21224" target="_blank" rel="noreferrer noopener">Hypertension</a></em>.<sup>10</sup> The effect was dose-dependent, which means those who drank more than one drink a day experienced greater increases in blood pressure over time.</p>
<!-- /wp:paragraph -->
<!-- wp:image {"id":834,"sizeSlug":"full","linkDestination":"none","align":"left"} -->
<figure class="wp-block-image alignleft size-full"><img src="https://medshadow.org/wp-content/uploads/2024/05/alch-300x300-1.png" alt="" class="wp-image-834"/><figcaption class="wp-element-caption"><em>Long-term use of alcohol can raise blood pressure</em></figcaption></figure>
<!-- /wp:image -->
<!-- wp:paragraph -->
<p>In the short term, indulging in a few drinks may temporarily lower your blood pressure by a few mm Hg, but about 13 hours later, you could see a slight increase in blood pressure. These effects are also dose-dependent. The amount of alcohol it takes to raise your blood pressure depends on your genetics, body composition and more, but it may be less than you think. A <a href="https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD012787.pub2/full" target="_blank" rel="noreferrer noopener">Cochrane review</a> showed that having more than two drinks was associated with a slight increase in blood pressure 13 hours later.<sup>11</sup><sup> </sup>The authors noted one caveat though, the individuals in the study were mostly healthy and male, so it’s possible that the findings don’t apply to everyone equally.</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":3} -->
<h3 class="wp-block-heading" id="h.er1rz57622zi">What is Resistant Hypertension?</h3>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p><a href="https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7415451/#:~:text=Resistant%20hypertension%20is%20defined%20by%20the%20American%20College%20of%20Cardiology%20and%20American%20Heart%20Association%20as%20blood%20pressure%20(BP)%20that%20remains%20above%20goal%20despite%20use%20of%20three%20maximally%20titrated%20anti%2Dhypertensive%20medications%20including%20a%20diuretic" target="_blank" rel="noreferrer noopener">Resistant hypertension</a><sup>12</sup> is high blood pressure that doesn’t seem to lower to the healthy range even after you’ve started exercising, changed your diet, and have taken blood pressure medications. It’s hypertension that persists with treatment.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>According to the American Heart Association, it’s likely that this type of hypertension has <a href="https://www.ahajournals.org/doi/10.1161/CIRCULATIONAHA.108.189141#d1e511" target="_blank" rel="noreferrer noopener">a secondary cause</a>,<sup>1</sup><sup>3</sup> some of which might not be addressed by the first-line treatments. Those causes could include sleep apnea, heavy drinking, hormonal imbalances and other conditions such as renal artery stenosis. If you have resistant hypertension, you may be prescribed multiple medications at the same time, and your blood pressure will need to be monitored more closely.</p>
<!-- /wp:paragraph -->
<!-- wp:heading -->
<h2 class="wp-block-heading" id="h.l2expxayjnm">How to Lower Blood Pressure</h2>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Before your doctor writes you a prescription for a blood-pressure-lowering drug, be sure to ask if lifestyle changes would be appropriate for you to try first.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>“There’s a difference between it being 146 over 80 and it being 170 over 80,” says <a href="https://wexnermedical.osu.edu/find-a-doctor/randell-wexler-md-12098" target="_blank" rel="noreferrer noopener">Randell Wexler,</a> MD, a primary care physician specializing in blood pressure control at the Ohio State University Wexner Medical Center. If your blood pressure is only a little elevated (in the range of 146 mm Hg/80 mm Hg, for example), Wexler suggests you could probably try lifestyle changes for six months to see if you can get it under control without medications. If your hypertension is more severe, such as 170 mm Hg/80 mm Hg, he says, you might need to start with medication, then add lifestyle changes and work with your clinician to see if you can eventually come off the medications.</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":3} -->
<h3 class="wp-block-heading" id="h.xttjrb4i79gr">Lifestyle Changes to Lower Your Blood Pressure</h3>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Eating a healthy diet with limited sodium, getting enough exercise, and managing stress are all crucial to helping lower your blood pressure.<sup>1</sup></p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":4} -->
<h4 class="wp-block-heading" id="h.daszgz7fxwdn">Foods to Lower Blood Pressure</h4>
<!-- /wp:heading -->
<!-- wp:image {"id":835,"sizeSlug":"full","linkDestination":"none","align":"left"} -->
<figure class="wp-block-image alignleft size-full"><img src="https://medshadow.org/wp-content/uploads/2024/05/sodium-300x300-1.png" alt="" class="wp-image-835"/><figcaption class="wp-element-caption">Choose low-sodium diet to lower your blood pressure<br></figcaption></figure>
<!-- /wp:image -->
<!-- wp:paragraph -->
<p>“At 80, my mother was released to hospice care with 10% heart function. Being too weak to go home, I brought her to my house,” says <a href="https://www.mamasezz.com/pages/founders-story" target="_blank" rel="noreferrer noopener">Meg Donahue</a>, referring to her mother, Millie. “After doing research, we decided to try changing her diet to a whole-food, plant-based diet. Because my mother was so weak, at first we fed her tiny smoothies and blended soups.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>“Over the next year, she gradually gained strength. And now, at the age of 88, her heart function and blood pressure are near normal. She swims four times a week, drives, and plays with her granddaughter daily,” adds Donahue. “It sounds like a miracle, but really the only miracle is we changed what she ate from foods that harm to foods that heal.”</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Reducing sodium is one strategy to lower blood pressure. If you’re trying to stick to a low-sodium diet, MedShadow’s guide to <a href="https://email.medshadow.org/sign-up-offer032021?_ga=2.150269426.510131833.1708465104-1520724301.1689595903&_gl=1*xmodob*_ga*MzkyMDc1NTMwLjE2MjMxNTc1ODg.*_ga_W9S7650GW0*MTcxMjA5Mzc1MS40ODcuMC4xNzEyMDkzNzUxLjYwLjAuMA.." target="_blank" rel="noreferrer noopener">Dining Out on a Low Sodium Diet</a> can help. Using a low sodium salt substitute is likely to help lower blood pressure slightly in adults, according to an <a href="https://www.cochrane.org/CD015207/PUBHLTH_does-using-low-sodium-salt-substitutes-lsss-instead-regular-salt-reduce-blood-pressure-and-heart" target="_blank" rel="noreferrer noopener">analysis of 26 studies</a>.<sup>14</sup> </p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Lowering the amount of sugar in your diet may slightly reduce your blood pressure, according to an <a href="https://www.cochrane.org/CD013320/VASC_low-levels-sugar-prevent-cardiovascular-disease" target="_blank" rel="noreferrer noopener">analysis of 21 trials</a>.<sup>15</sup> Dieting can also lead to weight loss, which can lower blood pressure if you carry extra weight. Melissa Finley lost 90 lbs, and when she was down by about 50, she says “My doc warned me, as we watched my weight drop, to be cautious of light-headedness when standing and other signs that my blood pressure was below where it should be.” When she started to have those symptoms, her doctor told her she could stop taking her blood pressure medication.</p>
<!-- /wp:paragraph -->
<!-- wp:embed {"url":"https://youtu.be/kRbbdDVKc9Q","type":"video","providerNameSlug":"youtube","responsive":true,"className":"wp-embed-aspect-16-9 wp-has-aspect-ratio"} -->
<figure class="wp-block-embed is-type-video is-provider-youtube wp-block-embed-youtube wp-embed-aspect-16-9 wp-has-aspect-ratio"><div class="wp-block-embed__wrapper">
https://youtu.be/kRbbdDVKc9Q
</div></figure>
<!-- /wp:embed -->
<!-- wp:heading {"level":3} -->
<h3 class="wp-block-heading">Exercise for Lowering Blood Pressure</h3>
<!-- /wp:heading -->
<!-- wp:image {"id":836,"sizeSlug":"full","linkDestination":"none","align":"right"} -->
<figure class="wp-block-image alignright size-full"><img src="https://medshadow.org/wp-content/uploads/2024/05/exercise-300x300-1.png" alt="" class="wp-image-836"/></figure>
<!-- /wp:image -->
<!-- wp:paragraph -->
<p>Exercise is also well-known to help control blood pressure. An <a href="https://www.cochrane.org/CD008823/HTN_effect-walking-blood-pressure-control" target="_blank" rel="noreferrer noopener">analysis of 73 trials</a><sup>16</sup> found that walking at a moderate intensity for as little as 20 to 40 minutes three to five times a week could lower systolic blood pressure.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>If you have hypertension, getting regular exercise can be just as effective at lowering your systolic blood pressure as taking medication, according to a large meta-analysis published in the <a href="https://bjsm.bmj.com/content/53/14/859.full" target="_blank" rel="noreferrer noopener">British Journal of Sports Medicine.</a><sup>17</sup></p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>While <a href="https://medshadow.org/exercise-for-different-diseases/" target="_blank" rel="noreferrer noopener">exercise is almost always helpful</a><a href="https://medshadow.org/exercise-for-different-diseases/" target="_blank" rel="noreferrer noopener"> for your health,</a> it’s important to talk to your healthcare provider before starting a new workout routine. In certain cases, you may need to start slowly and be on the lookout for signs you need to slow down or stop.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>To read more about walking and other exercises that can help lower your blood pressure check out <em>MedShadow’s:</em></p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p><a href="https://medshadow.org/podcasts-and-playlists/" target="_blank" rel="noreferrer noopener">Playlists and Podcasts to Power Your Next Walk or </a><a href="https://medshadow.org/podcasts-and-playlists/" target="_blank" rel="noreferrer noopener">Workout</a></p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p><a href="https://medshadow.org/tiktok-exercises/" target="_blank" rel="noreferrer noopener">TikTok Your Way to Fitness</a></p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p><a href="https://medshadow.org/water-aerobics/" target="_blank" rel="noreferrer noopener">Water Aerobics: A Safe Exercise for Many Patients</a></p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p><a href="https://medshadow.org/outdoor-workouts-when-you-dont-feel-like-running/" target="_blank" rel="noreferrer noopener">Outdoor Workouts for When You Don’t Feel Like Running</a></p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":4} -->
<h4 class="wp-block-heading" id="h.wldfq8m7pnm2">Stress Management for Blood Pressure Control</h4>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>There’s some truth to the old phrase “that gets my blood boiling!” Stress can <a href="https://www.heart.org/en/health-topics/high-blood-pressure/changes-you-can-make-to-manage-high-blood-pressure/managing-stress-to-control-high-blood-pressure" target="_blank" rel="noreferrer noopener">raise your blood pressure, at least in the short term</a>.<sup>18</sup> When you’re stressed, your body releases hormones that restrict your blood vessels, which, in turn, raises your blood pressure. When the stressor is no longer a threat (the tiger chasing you turns the other way or you finish your big presentation), your blood pressure should usually return to normal. There’s <a href="https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10961569/" target="_blank" rel="noreferrer noopener">some evidence</a><sup>19</sup> that chronic stress that doesn’t go away, for example stress associated with your daily work environment, can also raise your risk for hypertension.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Reducing stress can lower your blood pressure in the short term, and <a href="https://www.cochrane.org/CD004935/HTN_relaxation-for-high-blood-pressure-in-adults-which-has-no-clearly-identified-cause" target="_blank" rel="noreferrer noopener">possibly in the long term</a><sup>20</sup> as well. In an older review of 25 small trials, learning relaxation techniques such as progressive muscle relaxation reduced participant’s blood pressure, though the researchers pointed out that those who learned the techniques also may have had more contact with healthcare professionals than those who didn’t, which could have skewed the results.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>To read more about how to reduce stress to help lower your blood pressure check out <em>MedShadow’s:</em></p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p><a href="https://medshadow.org/forest-bathing-relax/" target="_blank" rel="noreferrer noopener">Can Forest Bathing Keep You Healthy?</a></p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p><a href="https://medshadow.org/yoga-for-health/" target="_blank" rel="noreferrer noopener">5 Ways Yoga Makes You Healthier</a></p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p><a href="https://medshadow.org/healthy-heart/" target="_blank" rel="noreferrer noopener">5 Lifestyle Changes to Maintain Heart Health</a></p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p><a href="https://medshadow.org/stress-management/" target="_blank" rel="noreferrer noopener">How to Manage Stress</a> </p>
<!-- /wp:paragraph -->
<!-- wp:image {"id":837,"sizeSlug":"full","linkDestination":"none","align":"left"} -->
<figure class="wp-block-image alignleft size-full"><img src="https://medshadow.org/wp-content/uploads/2024/05/sex-300x300-1.png" alt="" class="wp-image-837"/></figure>
<!-- /wp:image -->
<!-- wp:heading {"level":4} -->
<h4 class="wp-block-heading">Does masturbation lower blood pressure?</h4>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>As you might imagine, there isn’t a lot of scientific research on this topic. Nonetheless, sexual activities including masturbation, are similar to light or moderate cardiovascular workouts, so it’s reasonable to believe that regular masturbation could lower your blood pressure over time. Still, it’s not a substitute for other exercise and diet interventions.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p></p>
<!-- /wp:paragraph -->
<!-- wp:heading -->
<h2 class="wp-block-heading">9 Blood Pressure Medication Classes Chart</h2>
<!-- /wp:heading -->
<!-- wp:embed {"url":"https://youtu.be/BaqiXzrerJQ","type":"video","providerNameSlug":"youtube","responsive":true,"className":"wp-embed-aspect-16-9 wp-has-aspect-ratio"} -->
<figure class="wp-block-embed is-type-video is-provider-youtube wp-block-embed-youtube wp-embed-aspect-16-9 wp-has-aspect-ratio"><div class="wp-block-embed__wrapper">
https://youtu.be/BaqiXzrerJQ
</div></figure>
<!-- /wp:embed -->
<!-- wp:html -->
<script src="https://static-bundles.visme.co/visme-embed.js"></script>
<div class="visme_d" data-title="Types of bp medicines" data-url="g7qzog1w-types-of-bp-medicines" data-w="100%" data-full-h="true" data-h="100%" data-domain="my"></div>
<!-- /wp:html -->
<!-- wp:paragraph -->
<p></p>
<!-- /wp:paragraph -->
<!-- wp:heading -->
<h2 class="wp-block-heading" id="h.r6fjy525c8im">Side Effects of Blood Pressure Lowering Drugs </h2>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>According to an analysis of surveys, the <a href="https://jamanetwork.com/journals/jamaneurology/fullarticle/2768701" target="_blank" rel="noreferrer noopener">most frequently prescribed drugs</a><sup>21</sup> for high blood pressure from 2005 to 2016 were angiotensin-converting enzyme (ACE) inhibitors or angiotensin receptor blockers (59%) followed by beta-blockers (43.8%), and diuretics (35.7%). Less commonly used antihypertensive drugs were calcium channel blockers, alpha-blockers, and combined alpha- and beta-blockers. There is a newer drug, <a href="https://www.accessdata.fda.gov/drugsatfda_docs/label/2024/217686s000lbl.pdf" target="_blank" rel="noreferrer noopener">Tryvio (</a><a href="https://www.accessdata.fda.gov/drugsatfda_docs/label/2024/217686s000lbl.pdf" target="_blank" rel="noreferrer noopener">aprocitentan</a><a href="https://www.accessdata.fda.gov/drugsatfda_docs/label/2024/217686s000lbl.pdf" target="_blank" rel="noreferrer noopener">)</a>, that was approved in 2024 to be used alongside existing drugs to lower blood pressure. This medication works differently for treating hypertension than other drugs on the market.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>A large study published in <a href="https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/10.1001/jamainternmed.2024.0507?guestAccessKey=83a38214-8805-45b1-9f10-d190d69988fc&utm_source=For_The_Media&utm_medium=referral&utm_campaign=ftm_links&utm_content=tfl&utm_term=042224" target="_blank" rel="noreferrer noopener">JAMA</a><sup>22 </sup>in April 2024 found that nursing home residents who started any antihypertensive drug had an increased risk of falls and bone fractures requiring hospitalization. Patients with dementia or higher initial blood pressures had the greatest risk of experiencing a fall or fracture within 30 days of starting the medication.</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":3} -->
<h3 class="wp-block-heading" id="h.fx78i2d1g9hq"><a href="https://medshadow.org/need-to-know-ace-inhibitors/" target="_blank" rel="noreferrer noopener">Angiotensin Converting Enzyme (ACE) Inhibitors</a></h3>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>ACE inhibitors block angiotensin converting enzyme, which relaxes blood vessels to lower blood pressure. They also work to increase the amount of blood your heart pumps so that it doesn’t have to work as hard. Drugs from this class can help prevent additional tissue damage after you’ve had a heart attack.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Commonly used ACE inhibitors:</p>
<!-- /wp:paragraph -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>(lisinopril)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Accupril (quinapril)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Lotensin (benazepril)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Fosinopril</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Captopril</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Vasotec (enalapril)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Perindopril</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Altace (ramipril)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Trandolapril</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:heading {"level":4} -->
<h4 class="wp-block-heading" id="h.2ysh0q96siop">Side Effects of ACE Inhibitors</h4>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>A dry cough is a common<a href="https://medshadow.org/blood-pressure-hypertension-drugs/" target="_blank" rel="noreferrer noopener"> side effect</a> seen with ACE inhibitors. Occasionally, providers will prescribe a drug for reflux to treat the cough; it’s important to be aware of this possible <a href="https://medshadow.org/taking-too-many-drugs-you-may-be-in-a-prescription-cascade/" target="_blank" rel="noreferrer noopener">prescription cascade</a> and let your prescriber know you are taking an ACE inhibitor. Some people may experience dizziness or fainting if the drug causes their blood pressure to drop lower than it should. ACE inhibitors can also cause high potassium levels or stress the kidneys.<sup>23</sup></p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p><a href="https://www.nature.com/articles/s41440-023-01491-9" target="_blank" rel="noreferrer noopener">Swelling,</a><sup>24</sup> which can occur months or years after you start taking the drug, is another side effect of ACE inhibitors. It most commonly occurs around the eyes, tongue and throat. Depending on the severity of the swelling, you may need treatment before you stop taking the drug. When severe swelling occurs in the larynx, it can be life-threatening. Risk factors include being a woman, smoking, and a history of a cough caused by the drug. In <a href="https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10676215/" target="_blank" rel="noreferrer noopener">one instance</a>,<sup>2</sup><sup>5</sup> a woman experienced swelling in the intestine that caused nausea and vomiting that improved when she stopped taking the ACE inhibitor.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Other<a href="https://www.mayoclinic.org/diseases-conditions/high-blood-pressure/in-depth/ace-inhibitors/art-20047480?pg=2" target="_blank" rel="noreferrer noopener"> potential side effects</a> of ACE inhibitors:</p>
<!-- /wp:paragraph -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>Dizziness</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Irregular heart rhythm</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Elevated potassium levels</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:heading {"level":4} -->
<h4 class="wp-block-heading" id="h.g9724ggci6zo">Birth Defects</h4>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Taking ACE inhibitors during the <a href="https://mothertobaby.org/fact-sheets/ace-inhibitors-pregnancy/#:~:text=ACE%20inhibitors%20should%20be%20avoided,problems%20for%20the%20developing%20baby." target="_blank" rel="noreferrer noopener">second two trimesters of pregnancy</a><sup>26</sup> can raise the risk of birth defects in the baby. Ask your healthcare provider about using a different type of medication if you’re pregnant or hoping to become pregnant.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>For more information on these medications, review MedShadow’s “<a href="https://medshadow.org/need-to-know-ace-inhibitors" target="_blank" rel="noreferrer noopener">Everything You Need to Know About ACE Inhibitors</a>.”</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":3} -->
<h3 class="wp-block-heading" id="h.s81dc37xe328"><a href="https://medshadow.org/heart-health-meds-risks-v-benefits/#angiotensin" target="_blank" rel="noreferrer noopener">Angiotensin II Receptor Blockers</a> (ARBs)</h3>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Like ACE inhibitors, angiotensin II receptor blockers interfere with angiotensin to relax your blood vessels. They do this by blocking its receptors on the muscles surrounding blood vessels, which prevents the muscles from contracting.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Examples of ARBs include:</p>
<!-- /wp:paragraph -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>Edarbi (azilsartan)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Atacand (candesartan)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Teveten (eprosartan)</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:heading {"level":5} -->
<h5 class="wp-block-heading" id="h.12nlouve3kon">Birth Defects</h5>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>ARBs can <a href="https://www.ncbi.nlm.nih.gov/books/NBK537027/" target="_blank" rel="noreferrer noopener">cause birth defects</a><sup>27</sup> if you take them while you’re pregnant. If you could become pregnant, it is recommended to use <a href="https://medshadow.org/a-guide-to-contraception-and-side-effects/" target="_blank" rel="noreferrer noopener">contraception</a> while on these drugs. If you do become pregnant, your healthcare provider may have you switch to a different medication as soon as possible to keep your hypertension under control.</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":5} -->
<h5 class="wp-block-heading" id="h.ldilkbbgkxgw">Other possible side effects of ARBs include:</h5>
<!-- /wp:heading -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>Dizziness</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Low blood pressure</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>High potassium, which can cause abnormal heart rhythms, swelling, and even blocked airways.</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:heading {"level":3} -->
<h3 class="wp-block-heading" id="h.9audff4sl2fo"><a href="https://medshadow.org/heart-health-meds-risks-v-benefits/#beta" target="_blank" rel="noreferrer noopener">Beta Blockers</a> </h3>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Beta blockers interfere with adrenaline (also known as the hormone epinephrine) by blocking beta receptors on the heart, lungs, and other organs. Blocking adrenaline slows the heart rate and decreases the strength of heart-muscle contractions, minimizing how hard your heart works. This then lowers your blood pressure.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Examples of beta blockers include:</p>
<!-- /wp:paragraph -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>Toprol-XL (metoprolol)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Coreg (carvedilol)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Brevibloc (esmolol)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>bisoprolol</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:paragraph -->
<p>Healthcare providers may prescribe beta blockers after you’ve had a heart attack, especially if it caused heart failure.</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":4} -->
<h4 class="wp-block-heading" id="h.91h764tlbqvk">Side Effects of Beta Blockers</h4>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>If you have asthma, be sure to mention it to your cardiologist or other prescriber. People with asthma are at a higher risk of developing bronchospasm (increased asthma symptoms) while on beta blockers.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p><a href="https://www.ncbi.nlm.nih.gov/books/NBK532906/#:~:text=The%20blockade%20of%20these%20receptors,sexual%20dysfunction%20and%20erectile%20dysfunction." target="_blank" rel="noreferrer noopener">Other side effects</a><sup>28</sup> of beta blockers include the following:</p>
<!-- /wp:paragraph -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>Cold hands and feet (your blood isn’t reaching them as effectively.)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Fatigue</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Weight gain</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Dizziness</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Nausea and constipation</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Low blood pressure</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Low heart rate (bradycardia)</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>Headaches</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Erectile dysfunction or loss of sex drive</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Muscle and joint pain</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Shortness of breath or difficulty breathing (bronchial spasm)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Trouble sleeping and nightmares</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Depression</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Elevated blood sugar</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:heading {"level":3} -->
<h3 class="wp-block-heading" id="h.4no6z0z4faah"><a href="https://medshadow.org/heart-health-meds-risks-v-benefits/#diuretics" target="_blank" rel="noreferrer noopener">Diuretics</a> </h3>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Diuretics flush water and sodium out of your body, helping reduce the workload on your heart, which improves symptoms of heart failure and high blood pressure.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Here are some frequently used diuretics:</p>
<!-- /wp:paragraph -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>Lasix (furosemide)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Bumetanide</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Demadex (torsemide)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Diuril (chlorothiazide)</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Amiloride</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Chlorthalidone</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Hydrochlorothiazide</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Indapamide</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Metolazone</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Dyrenium (triamterene)</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:heading {"level":4} -->
<h4 class="wp-block-heading" id="h.7gi01b7o8x2g">Side Effects of Diuretics</h4>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>More frequent urination is a common side effect. It’s important to make sure you’re hydrated, especially when it’s<a href="https://medshadow.org/heat-sensitivity-side-effect/" target="_blank" rel="noreferrer noopener"> hot outside</a>. John Michael Sefel, a writer and researcher, told “MedShadow” that he went to the hospital more than once after experiencing headaches, dizziness and nausea due to the heat. He only recently learned that the diuretics he is taking may be putting him at risk.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Less common but serious side effects of diuretics include:</p>
<!-- /wp:paragraph -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>Dizziness</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Fainting</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li><a href="https://bmcpharmacoltoxicol.biomedcentral.com/articles/10.1186/s40360-024-00745-7" target="_blank" rel="noreferrer noopener">Kidney damage</a><sup>29</sup></li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Changes in levels of potassium, magnesium or calcium</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Uric acid buildup, which can cause gout</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:heading {"level":3} -->
<h3 class="wp-block-heading" id="h.1hppobqis33r">Endothelin Blocker</h3>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>The newest blood pressure drug, <a href="https://www.accessdata.fda.gov/drugsatfda_docs/label/2024/217686s000lbl.pdf" target="_blank" rel="noreferrer noopener">Tryvio</a> (aprocitentan) works by blocking the receptor for the hormone endothelin. This prevents the blood vessels from constricting. When your blood vessels are more relaxed, your blood pressure goes down. The drug was tested only in patients who still had uncontrolled blood pressure after having tried at least three other medications.</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":4} -->
<h4 class="wp-block-heading" id="h.fgp5m014g20u">Side Effects of Tryvio</h4>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Some patients experienced a small amount of <a href="https://medshadow.org/drugs-that-can-make-you-gain-weight/" target="_blank" rel="noreferrer noopener">weight gain</a> in the <a href="https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(22)02034-7/abstract" target="_blank" rel="noreferrer noopener">clinical trial</a>.<sup>30</sup> One of the more common side effects was swelling or fluid retention, which became more likely at higher doses. On the highest dose, 25 mg, about 18% of patients experienced fluid retention. The researchers treated the fluid retention with diuretics. Seven patients (out of 730) dropped out of the study due to swelling. This side effect of the medication was most common in people who also had chronic kidney disease.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Eleven patients in the study, ten of whom were taking the drug, were hospitalized with heart failure. The researchers suggested that this pointed to the importance of making sure that any patients with existing heart problems were having those problems properly managed before starting on Tryvio.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Another 11 patients died during the study: five from heart attacks, five from COVID, and one from an intestinal perforation that occurred during a medical procedure. The researchers did not believe these deaths were related to the treatment.</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":4} -->
<h4 class="wp-block-heading" id="h.ii0id0y4wz18">Birth Defects</h4>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Lastly, Tryvio is likely to <a href="https://www.accessdata.fda.gov/drugsatfda_docs/label/2024/217686s000lbl.pdf" target="_blank" rel="noreferrer noopener">cause birth defects</a> if taken during pregnancy. Make sure you’re using contraception if you’re taking this drug and could become pregnant, and let your provider know right away if a pregnancy occurs.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Since the drug was only FDA approved in March of 2024, we are likely to learn more about the side effects over the next few years. <a href="https://jamanetwork.com/journals/jama/fullarticle/2625319" target="_blank" rel="noreferrer noopener">Thirty-two percent</a><sup>31</sup> of drugs approved between 2001 and 2010 received a serious safety warning from the FDA, according to a 2017 study.</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":3} -->
<h3 class="wp-block-heading" id="h.beucurr2wlbh">Calcium Channel Blockers</h3>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>These drugs are prescribed to treat hypertension as well as a variety of other heart conditions and even migraines. Calcium makes your heart pump harder, and calcium channel blockers prevent calcium from entering cells in the heart and muscles, so the heart doesn’t work as hard to pump blood. That lowers your blood pressure.</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":4} -->
<h4 class="wp-block-heading" id="h.qwlaq8tijzx4">Side Effects of Calcium Channel Blockers</h4>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Calcium channel blockers can set off a common prescribing cascade. One of the frequent side effects of these drugs is edema or swelling. Rather than being recognized as a side effect, that symptom is often interpreted as a sign of a new condition by healthcare providers, according to a <a href="https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/2761272" target="_blank" rel="noreferrer noopener">2020 JAMA study</a>.<sup>32</sup> These patients are then prescribed diuretics to flush out the fluid causing the swelling.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Other <a href="https://www.ncbi.nlm.nih.gov/books/NBK482473/" target="_blank" rel="noreferrer noopener">side effects</a><sup>33</sup> can include any of the following:</p>
<!-- /wp:paragraph -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>Constipation</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Slowed heart rate</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Lightheadedness</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Flushing</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Headaches</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Swelling</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Inflamed gums</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:heading {"level":3} -->
<h3 class="wp-block-heading" id="h.rhxw5avcr97q">Alpha Blockers</h3>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Alpha blockers are occasionally used to treat hypertension, though they are typically not the first choice. They block alpha-1 receptors, leading to widening blood vessels that lower blood pressure. They generally aren’t meant to be used long-term.</p>
<!-- /wp:paragraph -->
<!-- wp:heading {"level":4} -->
<h4 class="wp-block-heading" id="h.h7ad2myn8dqu">Side Effects of Alpha Blockers</h4>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>People who have had cataract surgery should use caution when taking these drugs because they can cause problems with their eyes and irises.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>Other <a href="https://www.ncbi.nlm.nih.gov/books/NBK556066/" target="_blank" rel="noreferrer noopener">side effects</a><sup>34</sup> can include symptoms like these:</p>
<!-- /wp:paragraph -->
<!-- wp:list -->
<ul class="wp-block-list"><!-- wp:list-item -->
<li>Dizziness</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Fainting</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Falls</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Low blood pressure</li>
<!-- /wp:list-item -->
<!-- wp:list-item -->
<li>Rapid heart rate</li>
<!-- /wp:list-item --></ul>
<!-- /wp:list -->
<!-- wp:heading -->
<h2 class="wp-block-heading" id="h.v15656brp5mv">How Effective Are These Drugs in Lowering Blood Pressure?</h2>
<!-- /wp:heading -->
<!-- wp:paragraph -->
<p>Any reduction in blood pressure, whether you achieve it through lifestyle changes or the use of medication, lowers your risk of a variety of bad outcomes, such as heart attacks and strokes. A <a href="https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(15)01225-8/fulltext" target="_blank" rel="noreferrer noopener">meta-analysis of 123 trials</a><sup>35</sup> of different blood pressure-lowering drugs found that each 10 mm Hg reduction in systolic blood pressure (the top number) reduced the risk of major cardiovascular disease events by 20% (11.0% of those taking a placebo and 9.6% of those being treated had major cardiovascular disease), coronary heart disease by 17% (4.1% in the placebo group and 3.5% in the treated group had coronary heart disease), stroke by 27% (4.2% of those in the placebo group and 3.4% of those in the treated group had a stroke), heart failure by 28% (3.5% in the placebo group and 2.8% in the treated group had heart failure), and all-cause mortality by 13% (7.7% in the placebo group and 7.1% in the treated group died from any cause). The benefits from reducing the risk of kidney failure were less clear.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>The meta-analysis also found differences in the effectiveness of specific drug classes for preventing particular outcomes. For example, calcium channel blockers seemed most likely to prevent strokes, while diuretics were more likely to prevent heart failure. Medications were typically most effective for people who did not have chronic kidney disease or diabetes, though people with these conditions may still benefit from the treatments.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>The study is worth printing out and sharing with your provider as you discuss your individual risk level and treatment options, even though it does not include information on adverse effects or lifestyle changes.</p>
<!-- /wp:paragraph -->
<!-- wp:paragraph -->
<p>There are many options for managing high blood pressure. Both lifestyle changes and medications can play a role, but make sure you take the time to research the risks and benefits of each and discuss a detailed plan with your healthcare provider.</p>
<!-- /wp:paragraph -->