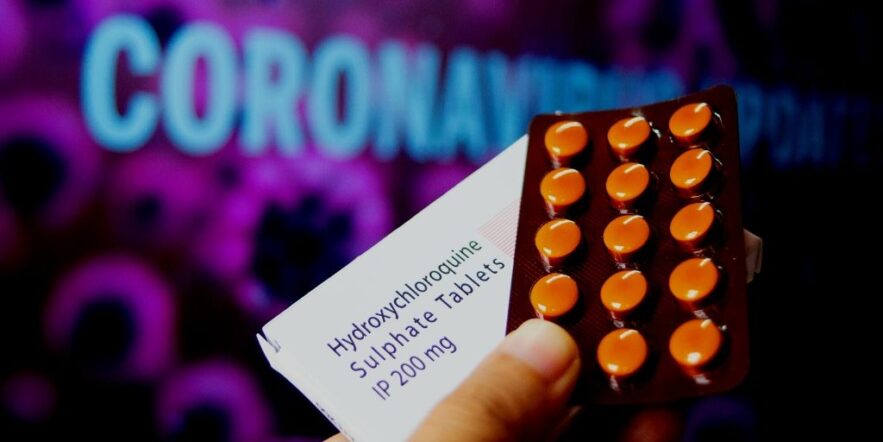
After months of speculation, clinical tests and a lot of hope, scientists reluctantly conclude that hydroxychloroquine is not the answer to COVID-19.
Hydroxychloroquine was identified early in the pandemic as one of several drugs that seemed likely to treat COVID-19. It was found to be effective against other coronaviruses in cell cultures which started the interest in hydroxychloroquine.
After months of testing and clinical trials, two strong, well-conducted studies have shown that hydroxychloroquine isn’t effective as a preventative for COVID-19 or as a way to treat it.
The study on preventative use of hydroxychloroquine was headed by researchers at the University of Minnesota and enrolled 821 adults who were asymptomatic in a randomized, double-blind placebo-controlled trial. Of this number, 87.6% of participants said they had a high-risk exposure to someone with confirmed COVID-19. Half the group was given hydroxychloroquine over a course of five days, while other participants were given a placebo to take over the same period. The primary outcome was confirmed COVID-19 or illness compatible with COVID-19 within 14 days of starting on active or placebo treatment.
Results showed there was no significant difference between the two groups in terms of new COVID-19 illnesses. About 12% of those on hydroxychloroquine developed COVID-19, compared to around 14% of those on the placebo. Side effects were much more common in the group given hydroxychloroquine – 40.1% vs 16.8% — compared to those in the placebo group. The most commonly reported side effects reported in the hydroxychloroquine group were nausea or stomach upset, diarrhea, abdominal comfort or vomiting, and neurologic reactions such as irritability, dizziness and vertigo.
Researchers concluded that the trial “did not demonstrate a significant benefit of hydroxychloroquine as postexposure prophylaxis for COVID-19.”
Martin Landray, PhD, professor of medicine and epidemiology at the Nuffield Department of Population Health at Oxford University, notes that the relatively small number of participants makes the results far from definitive. “The study makes it very unlikely that there is a large effect (e.g. a halving in the risk of infection) but cannot rule out a more modest difference (e.g. a reduction of one-quarter or one-third) which would still be very valuable.”
It’s important to note that this study was not designed to evaluate whether hydroxychloroquine is safe and effective as a treatment for those already sick with COVID-19.
New significant research indicates that hydroxychloroquine also does not help treat patients with COVID-19. Investigators with a major UK trial that has enrolled over 11,000 hospitalized COVID-19 patients examining various drug treatments last week said they will stop enrolling patients in the hydroxychloroquine arm because of a lack of beneficial effect.
Preliminary results of more than 1500 patients dosed with hydroxychloroquine showed that after 28 days, there was no significant difference in mortality between the hydroxychloroquine group and the usual care group. Results showed 25.7% of those on hydroxychloroquine died compared to 23.5% receiving usual care.
Landray, who is one of the primary investigators in this trial, dubbed RECOVERY, commented, that the results indicate that “hydroxychloroquine does not reduce the risk of death among hospitalized patients with this new disease. This result should change medical practice worldwide and demonstrates the importance of large, randomized trials to inform decisions about both the efficacy and safety of treatments.”